When to See a Lactation Consultant

When to See a Lactation Consultant
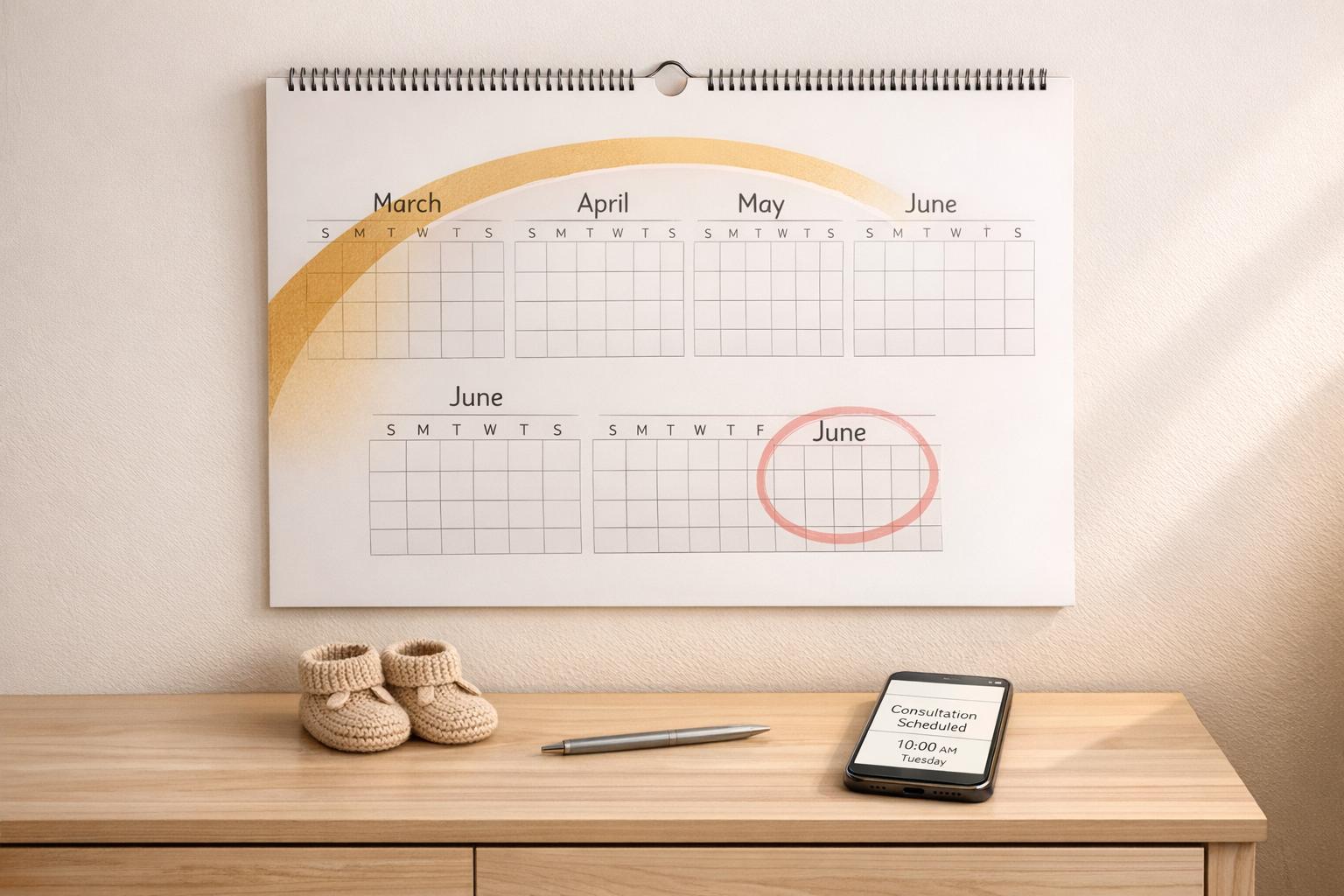
Breastfeeding can be challenging, especially in the early days. A lactation consultant can help with issues like latching, milk supply, nipple pain, or feeding plans for premature babies. The first 24–72 hours postpartum are critical for establishing breastfeeding, and early support can make a big difference. These professionals also provide emotional support, guidance on hunger cues, and advice on feeding techniques. If you experience ongoing pain, your baby isn’t gaining weight, or you have health conditions affecting milk production, seeking help promptly is important. Many insurance plans cover lactation services, making them more accessible for families.
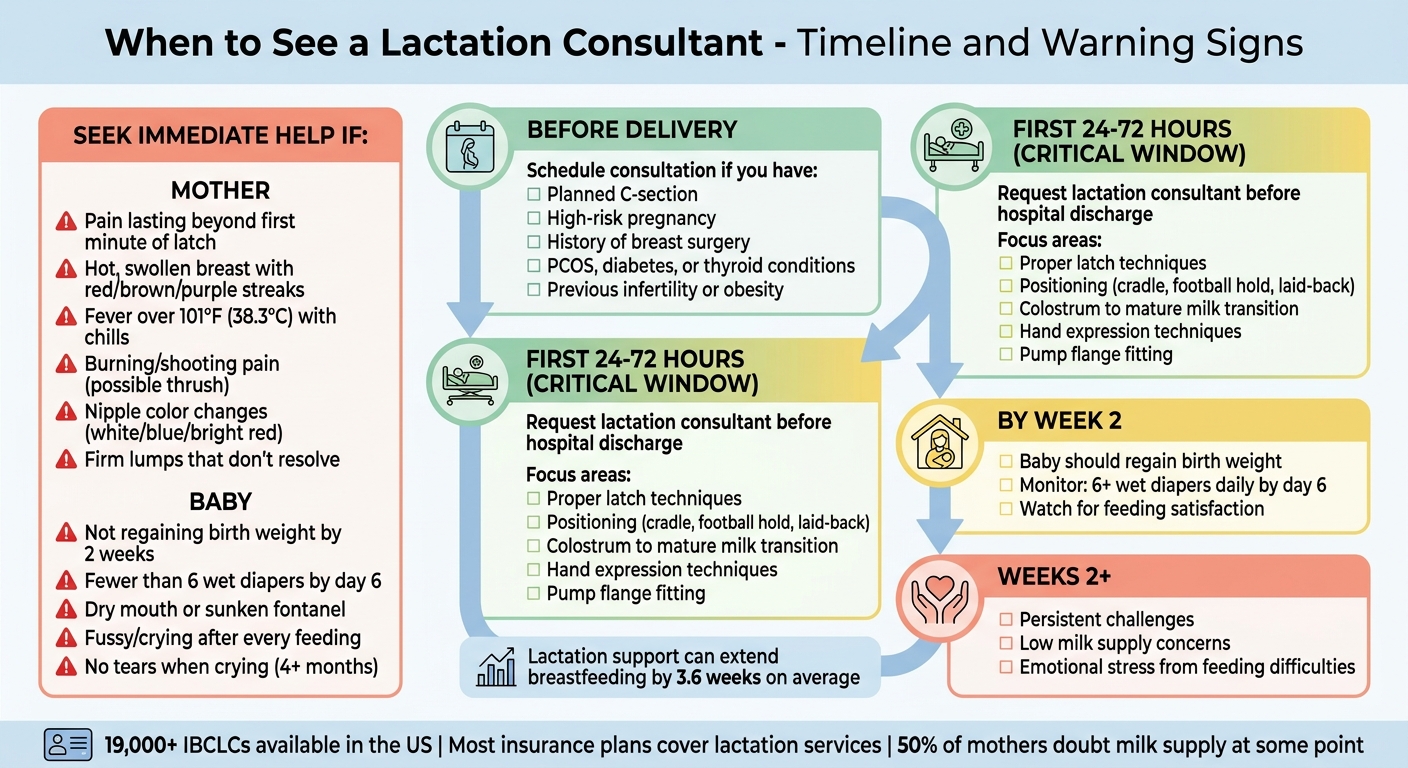
When to See a Lactation Consultant: Timeline and Warning Signs
Signs You Should See A Lactation Consultant
sbb-itb-9ce2258
When to See a Lactation Consultant in the First Few Days After Birth
The first few days after giving birth are crucial for establishing breastfeeding. Even if things seem to be going well while you're still in the hospital, small issues can quickly escalate once you're home. This is the time when proper positioning and latch techniques become essential for both you and your baby.
"You might need this support most urgently during the first few weeks of your baby's life. This is when your baby is learning how to nurse, and both of you may need more support." - Cleveland Clinic
If you're delivering in a hospital, make sure to ask for a lactation consultant visit before you're discharged. Use this opportunity to discuss common concerns like nipple pain, how long nursing sessions should last, and how to tell if your baby is getting enough milk.
Getting a Proper Latch and Starting Milk Production
A good latch is the foundation of comfortable and effective breastfeeding. If your baby is having trouble latching, a lactation consultant can step in to correct it right away. They'll guide you through different breastfeeding positions - such as cradle, cross-cradle, football hold, or laid-back breastfeeding - and show you how to help your baby achieve a deep, comfortable latch.
In the first 72 hours, your body transitions from producing colostrum to mature milk. A consultant can help identify any challenges - whether hormonal, physical, or emotional - that might affect your milk supply. They’ll also teach you hand expression techniques to collect colostrum or relieve engorgement. If you're using a breast pump, they'll ensure the flange fits properly to maximize milk removal and minimize discomfort.
Tracking your baby's milk intake can feel daunting, but lactation consultants simplify the process. They’ll teach you how to use diaper counts as a reliable way to monitor milk transfer. Some also use specialized scales to measure your baby’s weight before and after feedings, giving you a clear picture of how much milk your baby is taking in.
For those recovering from a challenging delivery, consultants can tailor their support to your specific postnatal care needs.
Breastfeeding After a C-Section or Difficult Birth
If you’ve had a C-section, finding a comfortable nursing position is essential. A consultant can recommend positions like the football hold or laid-back method, which help protect your incision while ensuring your baby can nurse effectively.
"A lactation consultant can help you navigate any number of new baby feeding challenges, including... struggles with finding the right nursing position, especially after a C-section." - Catherine Donaldson-Evans
Complicated births, such as those requiring NICU stays or involving premature babies, can sometimes delay milk production. In these cases, lactation consultants create customized feeding plans to support babies who may not yet have the coordination to suck, breathe, and swallow properly. They also address the physical recovery and emotional stress that can make breastfeeding more challenging. Studies show that working with a lactation consultant can extend breastfeeding by an average of 3.6 weeks and reduce the likelihood of stopping exclusive breastfeeding by 4%.
If you’re planning a scheduled C-section or have a high-risk pregnancy, meeting with a consultant before delivery can be incredibly helpful. They can help you prepare a plan for early milk expression or pumping, making the first few days after birth much easier.
Getting early support from a lactation consultant can prevent feeding difficulties and help ensure a healthy milk supply for your baby.
Signs You Need Immediate Lactation Support
Recognizing when to seek help with breastfeeding can make a big difference. While some discomfort is common during the early days, certain symptoms shouldn't be ignored and may require quick attention from a lactation expert.
Breast Pain or Discomfort During Feeding
It's normal to feel some sensitivity at first, but sharp or ongoing pain is a red flag. If breastfeeding hurts beyond the first minute of a latch, it's time to get help.
"If breastfeeding hurts for more than the first minute of a latch, something is wrong." - Milky Mama
Other warning signs include a breast that feels hot, swollen, or painful, especially if there are red streaks. On darker skin, these streaks might look like brown or purplish patches. These symptoms could indicate mastitis, particularly if accompanied by a fever over 101°F (38.3°C), chills, body aches, or fatigue. In such cases, medical attention is crucial.
A sudden burning or shooting pain after weeks of pain-free nursing could mean thrush, a fungal infection. Similarly, if your nipple changes color - turning white, blue, or bright red after feeding or exposure to cold - and is accompanied by sharp pain, vasospasm might be the cause. Firm, tender lumps that don’t go away with feeding or gentle massage could signal a blocked duct or early mastitis. If pumping remains painful despite adjustments, it's worth consulting a lactation specialist.
These symptoms, combined with feeding difficulties, highlight the importance of seeking timely lactation support.
Baby's Weight Loss or Feeding Problems
Your baby's feeding habits and weight can also signal potential breastfeeding challenges.
It's normal for newborns to lose some weight in the first few days, but they should regain their birth weight by about two weeks. If your baby isn't gaining weight steadily after this period, a professional evaluation is recommended.
By day six, your baby should have at least six wet diapers daily. Watch for signs of dehydration, such as a dry mouth or a sunken fontanel. For babies older than four months, a lack of tears when crying can also indicate dehydration.
Pay attention to how your baby behaves after feeding. A content baby often looks relaxed or "milk drunk." On the other hand, if your baby remains fussy, continues crying, or shows rooting behavior (searching for the breast) right after feeding, they may not be getting enough milk. Sometimes, this happens due to a poor latch, which can prevent effective milk removal even if your supply is sufficient.
"Sometimes, you can make plenty of milk, but the baby can have issues physically pulling the milk from the breast." - Kristin Barrett, MD, Pediatrician, Cleveland Clinic
If you're pumping and notice low milk output, check the pump's components, especially the valves, as mechanical issues might be to blame rather than a true low supply. A lactation consultant can also perform a weighted feed to determine exactly how much milk your baby is getting during nursing.
Catching these issues early can help maintain a healthy milk supply and ensure your baby is well-fed.
Maternal Health Conditions That May Require Lactation Support
Your medical history can play a big role in breastfeeding success. Some conditions can interfere with the hormonal signals needed for milk production, making early professional help essential.
Medical History and Health Concerns
Certain pre-existing conditions can lead to low milk supply. For example, Type 1 or Type 2 diabetes, insulin resistance, and thyroid issues may delay or even prevent the transition to full milk production, which usually occurs around the third day after giving birth.
Polycystic Ovarian Syndrome (PCOS) is another condition that can disrupt the hormonal balance required for lactation. Maureen Anderson, CNM, DNP, MST, a Certified Nurse Midwife and IBCLC at Providence, explains:
"There are people who physically have a more difficult time either because of a lack of tissue that will produce milk, or a hormonal condition such as polycystic ovarian syndrome (PCOS)."
Women with a history of infertility or obesity may also face a higher likelihood of milk supply challenges.
If you've had breast surgeries - such as reductions, augmentations, or biopsies - these procedures may have affected milk ducts or glandular tissue. If this applies to you, consider scheduling a consultation during pregnancy to create a personalized feeding plan.
Interestingly, about 50% of breastfeeding mothers doubt their ability to produce enough milk at some point. A lactation consultant can help separate actual supply issues from perceived ones by monitoring your baby's weight gain and diaper output.
Postpartum Recovery Challenges
Complications during or after childbirth can also impact milk production. For instance, a retained placenta or significant postpartum bleeding can lower prolactin levels, which are vital for milk production. Normally, the delivery of the placenta triggers the hormonal changes that initiate lactation, so any disruption in this process may require professional evaluation.
Additionally, certain medications used to treat postpartum health issues - especially those containing estrogen or pseudoephedrine - can reduce milk supply. If you're taking medications, a lactation consultant can review them and suggest alternatives when appropriate. Simple techniques like applying moist heat for 3–5 minutes before feeding and practicing skin-to-skin contact can help stimulate milk release and boost oxytocin levels.
Breastfeeding also provides long-term health benefits for mothers, including a 30% to 40% lower risk of developing Type 2 diabetes later in life.
When Breastfeeding Problems Continue Beyond the First Few Weeks
While many early breastfeeding challenges improve with time and support, some struggles persist or even emerge later on. It's common to expect breastfeeding to become smoother after the initial adjustment period, but that isn't always the case. If you're still facing difficulties weeks or months into your journey, it might be time to reach out for professional guidance. As Carrie Dean, IBCLC and Founder of Mama Bear Dean, puts it:
"Breastfeeding is natural, but it's a very intricate dance between two human bodies. One little bump can cascade into big concerns quickly."
Low Milk Supply or Feeding Pattern Problems
Signs like stalled weight gain, fewer than six wet diapers daily, or a baby who remains fussy and seems unsatisfied after feeding could signal insufficient milk intake. If your baby hasn’t regained their birth weight by the two-week mark, it’s worth seeking expert advice.
An International Board Certified Lactation Consultant (IBCLC) can help identify the root of the issue. Whether it’s an ineffective latch, true milk supply concerns, or feeding challenges - like a newborn who struggles to stay awake or an older baby who gets easily distracted - an IBCLC can assess your unique situation and offer tailored solutions. With over 19,000 IBCLCs practicing in the United States, support is accessible both in person and through telemedicine platforms like Zoom or FaceTime.
Struggles with feeding not only affect your baby but can also chip away at your confidence as a parent, making emotional support just as important as technical help.
Emotional Stress from Breastfeeding Difficulties
When physical challenges linger, the emotional impact can make breastfeeding feel even harder. It’s normal to feel frustrated, anxious, or discouraged when the process doesn’t match your expectations. Instead of waiting for things to reach a breaking point, consider seeking help - not just for guidance but for the reassurance that you’re not alone.
Carrie Murphy, Doula and Writer, highlights the emotional benefits of seeking support:
"Seeking lactation help not only makes for a better breastfeeding relationship, it also expands and improves your overall emotional support system - a necessity for any new mom."
The Cleveland Clinic echoes this sentiment:
"They'll offer expert guidance - and sometimes simply a listening ear - to help you navigate this time."
If breastfeeding feels overwhelming, connecting with a professional can provide both practical strategies and the emotional comfort you need to continue your journey for as long as you choose.
How Nestling Can Help with Professional Lactation Support
Getting professional lactation support shouldn’t be a waiting game. With Nestling, families can connect with certified IBCLCs (International Board Certified Lactation Consultants) through on-demand telehealth appointments available every day of the week. These experts are certified by the International Board of Lactation Consultant Examiners, ensuring they bring a high level of training and expertise.
Nestling tailors its support to meet the specific needs of new parents during the early postpartum period. Consultants review your health history, postpartum recovery needs, and your baby’s feeding patterns, observe feedings during the session, and provide hands-on coaching. Whether you’re dealing with nipple pain, figuring out the right fit for your breast pump, or learning to recognize your baby’s hunger signals, Nestling’s IBCLCs are there to guide you.
One parent shared their experience:
"My IBCLC validated my experience, supported, and encouraged me in my breastfeeding and pumping efforts. She helped me remember rest and stability are just as important as milk production."
Nestling is widely praised for its contributions to pediatric health. Many families find that most appointments come with no out-of-pocket costs under commercial health insurance. For those on Medicaid or without insurance, Nestling offers discounted rates. To make the service even more accessible, bilingual consultants are available, so families can receive help in the language they’re most comfortable with.
Beyond solving immediate feeding concerns, Nestling’s consultants work closely with your primary care team to ensure everyone is on the same page about your care plan. Whether you’re figuring out how to remove milk effectively, setting up a manageable pumping schedule, or working feeding goals into your daily life, Nestling provides expert advice and emotional support. Their guidance not only addresses current challenges but also helps lay the foundation for long-term breastfeeding success.
Conclusion
Reaching out for lactation support at the right time can make a big difference in your breastfeeding journey. The early days are especially important for getting breastfeeding on track, and addressing concerns like nipple pain, latching issues, or questions about your baby’s weight gain early can prevent these manageable challenges from turning into bigger hurdles that could impact your experience. Seeking help early ensures you get expert guidance when it matters most.
Certified IBCLCs offer more than just practical advice - they provide much-needed emotional support during what can be a vulnerable time. Dr. Marieme Mbaye, an ob-gyn, highlights the importance of their role:
"As an ob-gyn, I've seen so many new parents struggle to figure out breastfeeding for themselves and their babies... Their insights can be priceless during this adjustment period".
Carrie Dean, IBCLC, also stresses the importance of acting quickly when challenges arise:
"One little bump can cascade into big concerns quickly. Having a complete, skilled assessment of the [mother-child] dyad will allow the IBCLC to develop a tailored plan to help keep everyone on their optimal path. Don't wait to get help!".
These expert perspectives make it clear: timely lactation support is essential for a successful breastfeeding journey. From resolving specific issues to providing reassurance, lactation consultants play a critical role. Research shows that lactation support increases the chances of sustained breastfeeding. With over 19,000 IBCLCs available across the United States and many insurance plans covering these services under the Affordable Care Act, getting professional help has never been more accessible. Early intervention can transform challenges into a rewarding and empowering breastfeeding experience.
FAQs
Is my low milk supply real or just perceived?
Low milk supply is often more of a concern than a reality. For instance, having softer breasts after the initial engorgement phase or a baby waking up frequently doesn’t necessarily mean your milk supply is low. True low supply is usually identified by more concrete signs, like poor weight gain in your baby or very little active swallowing during feeding sessions. If you’re feeling uncertain, reaching out to a lactation consultant can provide clarity and support.
How can I tell if my baby is getting enough milk?
You can tell if your baby is getting enough milk by keeping an eye on their weight gain, tracking the number of wet diapers, and watching for any signs of dehydration. Dehydration might show up as fewer wet diapers than usual or unusual lethargy. If you’re worried, reach out to a healthcare provider or a lactation consultant for advice.
When should I see an IBCLC versus my doctor?
Seeing an IBCLC (International Board Certified Lactation Consultant) can make a big difference when you’re facing breastfeeding challenges like latch issues, nipple pain, or concerns about low milk supply. These specialists offer personalized support and can start helping as early as 24–72 hours after your baby is born. While your doctor oversees your overall postpartum health, an IBCLC zeroes in on breastfeeding, making them the go-to resource for tricky situations or important moments, such as preparing to return to work or navigating your baby’s growth spurts.