Sleep Deprivation and Postpartum Depression

Sleep Deprivation and Postpartum Depression
Sleep deprivation and postpartum depression are closely linked, creating a cycle that can deeply impact new mothers. Lack of sleep disrupts hormones like serotonin and dopamine, increasing the risk of depression. At the same time, postpartum depression can worsen sleep problems, leading to ongoing exhaustion and emotional struggles.
Key Points:
- Over 66% of new mothers experience poor sleep in the first six months postpartum.
- Chronic sleep loss raises the risk of postpartum depression by more than 3 times.
- Symptoms of sleep deprivation and postpartum depression often overlap, making it hard to identify the root cause.
- Warning signs of postpartum depression include persistent sadness, difficulty bonding with the baby, and feelings of guilt or hopelessness.
Solutions to Break the Cycle:
- Prioritize uninterrupted 4–6 hour sleep blocks with partner or caregiver support.
- Create a sleep-friendly environment: cool room (65–68°F), blackout curtains, and white noise.
- Seek professional help if symptoms persist, such as postpartum doulas or therapy like CBT-I.
- Build a support network and divide responsibilities to reduce stress.
If you're feeling overwhelmed, it's important to act early. Addressing sleep issues and seeking help can protect your mental health and strengthen your connection with your baby.
Sleep Deprivation After Pregnancy | How much sleep should mom get? | Sleep Deprived Postpartum
sbb-itb-9ce2258
Sleep Deprivation in New Mothers
Sleep deprivation occurs when your body and mind consistently function below their normal levels due to insufficient or poor-quality sleep. For new mothers, this isn't just an occasional issue - it becomes a daily reality. In fact, over 66% of individuals who give birth report poor sleep quality during the first six months postpartum. And the effects go far beyond mere tiredness. Let’s dive into the biological and practical reasons behind this sleep loss.
What Causes Sleep Deprivation After Childbirth
The sleeplessness experienced by new mothers stems from a mix of biological changes and practical challenges. Hormonal shifts are a major factor. After childbirth, levels of progesterone - a hormone that aids in deep, restful sleep - plummet. At the same time, estrogen levels drop to levels similar to those seen during menopause. Dr. Alyssa Dweck, a gynecologist, explains:
"Low estrogen levels postpartum can mirror menopausal levels and cause hot flashes and night sweats, which can disrupt sleep quantity and quality".
For breastfeeding mothers, elevated prolactin levels further disrupt sleep cycles, making rest lighter and less restorative. Add to this the reality of a newborn’s feeding schedule - every 2–3 hours - and it becomes nearly impossible to complete a full 90-minute sleep cycle, which is essential for deep, restorative rest. These constant interruptions also throw off your circadian rhythm.
Physical discomfort adds another layer of difficulty. Whether it’s pain from childbirth recovery, soreness from breastfeeding, or muscle tension from holding and feeding your baby, these physical demands make it even harder to get quality rest. Recognizing these factors is crucial for addressing the cycle of sleep deprivation and its broader effects on health. Many families find that postpartum doula support can help manage these challenges during the early weeks.
These disruptions not only affect sleep patterns but also trigger a cascade of physical and emotional challenges.
How Sleep Loss Affects Physical and Mental Health
The consequences of chronic sleep deprivation go far beyond feeling tired. A study conducted by UCLA in August 2021 found that mothers who slept less than seven hours per night at six months postpartum had a biological age three to seven years older than those who got at least seven hours. This was linked to shortened telomeres in their white blood cells, a marker associated with an increased risk of age-related diseases.
Professor Judith Carroll, the study’s lead researcher, emphasized:
"The early months of postpartum sleep deprivation could have a lasting effect on physical health. We know from a large body of research that sleeping less than seven hours a night is detrimental to health and increases the risk of age-related diseases".
On the mental health side, chronic sleep loss disrupts the balance of serotonin and dopamine, increasing vulnerability to depression. Persistent sleep deprivation also keeps cortisol - the stress hormone - elevated, leading to a constant state of low-grade stress. This heightened stress not only worsens anxiety but also interferes with oxytocin, the hormone essential for bonding with your baby. To make matters worse, sleep-deprived mothers often experience impaired functioning of the prefrontal cortex, making it harder to manage overwhelming emotions or racing thoughts, all of which heighten the risk of postpartum depression.
Postpartum Depression: Symptoms and Warning Signs
Sleep Deprivation vs Postpartum Depression: Symptom Comparison Guide
Sleep deprivation can take a serious toll on cognitive and emotional well-being, but it’s important to recognize when those struggles might signal something deeper, like postpartum depression (PPD). Did you know that 1 in 5 new mothers experiences postpartum depression within the first six months after giving birth? Unlike the "baby blues" - a common experience for up to 80% of new moms that usually resolves within two weeks - PPD is more severe and long-lasting. Spotting the warning signs early is key, especially since PPD symptoms often overlap with the effects of extreme sleep deprivation.
Common Symptoms of Postpartum Depression
Postpartum depression can feel like being stuck in a fog of constant sadness, hopelessness, or apathy. Some common signs include:
- Loss of appetite
- Irritability or hostility toward loved ones
- Persistent self-blame and low self-esteem
- Difficulty bonding with your baby, which sets PPD apart from simple exhaustion
The intensity of symptoms varies. For some, it’s a mild disruption to daily life, while for others, it can be so overwhelming that even basic self-care or caring for their baby becomes unmanageable. If emotional symptoms last more than two weeks, it’s time to reach out to a healthcare provider - whether that’s your OB, midwife, or a mental health professional. And if you’re experiencing thoughts of harming yourself or your baby, or feeling disconnected from reality, seek help immediately.
Symptoms That Overlap Between Sleep Deprivation and Postpartum Depression
One challenge in identifying PPD is that it shares many symptoms with sleep deprivation. Both can cause extreme irritability, trouble concentrating, feelings of being emotionally overwhelmed, and physical exhaustion. This overlap can make it tricky for moms - and even healthcare providers - to pinpoint what’s truly going on. Recognizing both shared and unique symptoms is essential for getting the right support.
Here’s a quick comparison of how sleep deprivation and PPD might present:
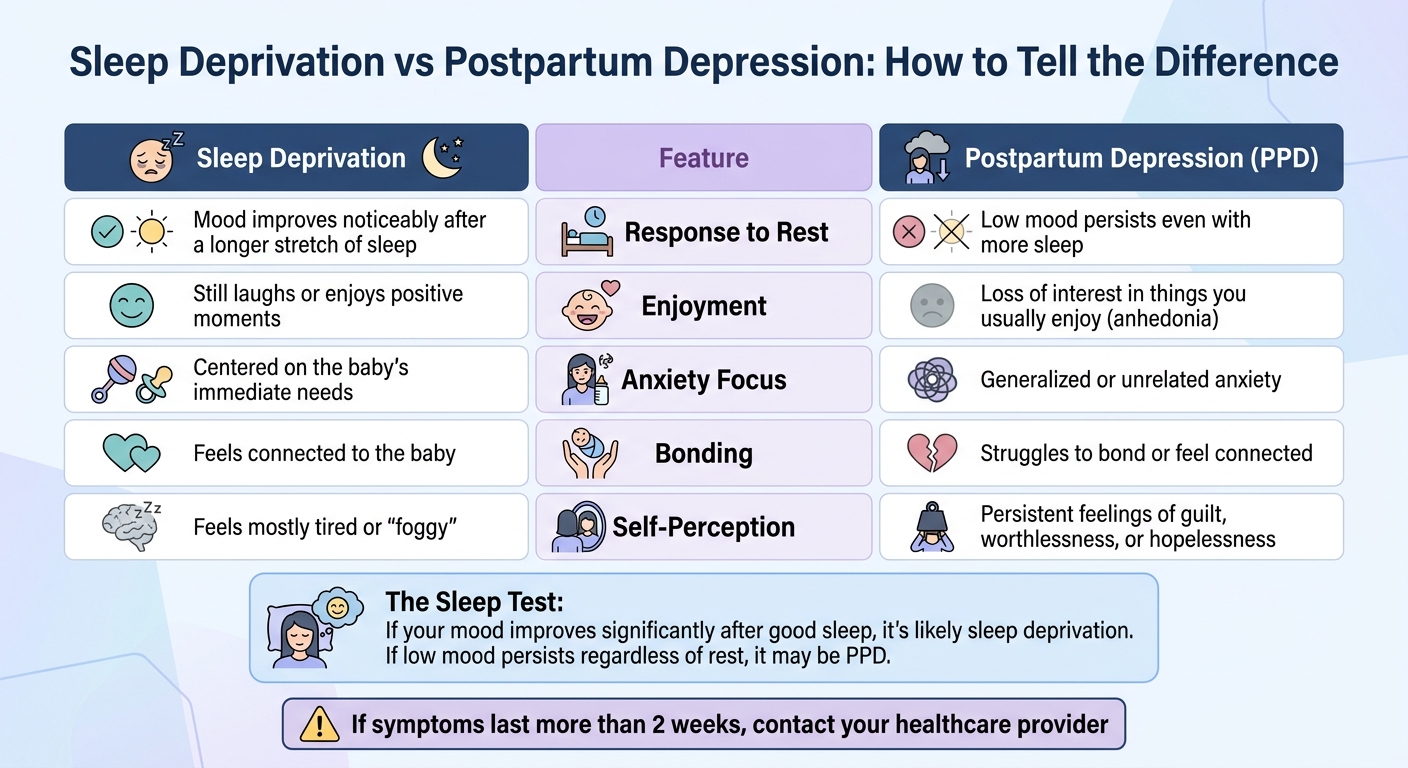
| Feature | Points Toward Sleep Deprivation | Points Toward PPD |
|---|---|---|
| Response to Rest | Mood improves noticeably after a longer stretch of sleep | Low mood persists even with more sleep |
| Enjoyment | Still laughs or enjoys positive moments | Loss of interest in things you usually enjoy (anhedonia) |
| Anxiety Focus | Centered on the baby’s immediate needs | Generalized or unrelated anxiety |
| Bonding | Feels connected to the baby | Struggles to bond or feel connected |
| Self-Perception | Feels mostly tired or “foggy” | Persistent feelings of guilt, worthlessness, or hopelessness |
A helpful tool is the "sleep test": if your mood improves significantly after a good stretch of sleep, the issue is likely sleep deprivation. But if your mood remains low regardless of rest, it’s a sign of PPD. Another red flag? If you can’t sleep even when the baby is sleeping due to racing thoughts or anxiety. This often signals PPD rather than just exhaustion.
Understanding these differences matters, especially as we dive deeper into how sleep loss and PPD can feed into each other in the next section.
How Sleep Deprivation and Postpartum Depression Feed Each Other
Sleep deprivation and postpartum depression don’t just coexist - they fuel one another in a cycle that can feel impossible to escape. Chronic lack of sleep disrupts the production of serotonin and dopamine, two key neurotransmitters often targeted by antidepressants. On top of that, it keeps cortisol - your stress hormone - elevated, which lowers your ability to handle anxiety and interferes with oxytocin, the hormone that plays a vital role in bonding. Together, these changes create the perfect storm for emotional and mental challenges.
When postpartum depression sets in, it further undermines sleep, locking you into a self-reinforcing loop. Anxiety can make it harder to fall asleep, leaving you with racing thoughts or a sense of dread about the next wake-up. It can also cause you to wake up in the early hours, unable to fall back asleep despite feeling utterly drained. Depression, meanwhile, disrupts your sleep cycles, so even when you do manage to sleep, it’s often not restorative.
Studies show just how closely linked sleep and postpartum depression are. Poor sleep quality increases the risk of postpartum depression by over three times. Additionally, a mother’s sleep quality at six months postpartum is a strong predictor of her mood at the one-year mark. The longer this cycle continues, the tougher it becomes to break free.
That’s why early action is so important. If your mood doesn’t improve even after a rare stretch of uninterrupted sleep, or if nighttime anxiety worsens as evening approaches, these could be warning signs that the cycle is taking hold. The encouraging news? This pattern can be disrupted. Strategies like scheduling protected sleep blocks, enlisting help from partners or caregivers, and seeking professional support if symptoms persist beyond two weeks can make a world of difference. Acting early not only safeguards your mental health but also strengthens the bond with your baby.
Practical Solutions for Better Sleep and Mental Health
Sleep Habits and Routines for New Mothers
Caring for a newborn can make sleep feel like a luxury, but there are ways to make the most of your rest. Try using split-sleep schedules with a partner or caregiver to secure one uninterrupted 4–6-hour block of sleep. This kind of consolidated rest is far more rejuvenating than several short naps scattered throughout the day.
Your sleep environment matters, too. Keep your room between 65°F and 68°F, use blackout curtains to block out light, and consider a white noise machine to mask disruptions. Dimming lights and avoiding screens 30–60 minutes before bedtime can also support melatonin production, helping you fall asleep faster.
Another tip? Let go of the urge to tackle household chores when your baby naps. Use that time for your own rest instead. Even a short morning walk in the sunlight can reset your body’s internal clock, improving your alertness and regulating your sleep patterns.
If these steps still aren’t enough, seeking professional postpartum support can make a big difference.
Getting Professional Postpartum Help
Sometimes, adjusting your sleep habits isn’t enough to fully recover from sleep deprivation. That’s where professional help comes in. Overnight caregivers, like postpartum doulas or night nurses, can step in to handle nighttime feedings, giving you the chance to get a solid 4–5 hours of uninterrupted sleep. This can be a game-changer, especially since only about 10% of parents manage to get the recommended 7 or more hours of sleep per night after having a baby, compared to 68% before.
Services like Nestling connect families with trusted postpartum professionals, including doulas, lactation consultants, and infant care specialists. These caregivers provide overnight care, feeding assistance, and emotional support, all tailored to your needs. Lactation consultants, in particular, can help resolve breastfeeding challenges, which are often linked to postpartum depression.
Therapy Options for Postpartum Depression
If improving sleep habits and seeking professional help aren’t enough, therapy can offer further relief. Cognitive Behavioral Therapy for Insomnia (CBT-I) is highly effective, with success rates ranging from 60% to 70%. This approach focuses on reducing the anxiety around sleep, especially the pressure to "sleep when the baby sleeps", which can sometimes cause even more stress.
"The gold standard for treatment is cognitive behavioural therapy (CBT). This should always be the first line of defense".
For those experiencing moderate to severe postpartum depression, addressing sleep alone might not suffice.
"CBTi is the gold standard for the treatment of insomnia and has consistently been shown to improve symptoms of depression".
Research shows that women with poor sleep quality are 3.34 times more likely to develop postpartum depression than those who sleep well.
Mindfulness practices, such as Yoga Nidra, body scans, and guided meditations, can also help calm your nervous system. Setting aside 15–20 minutes for low-stimulation activities - like gentle stretching in dim lighting - before bed can signal to your body that it’s time to wind down. Digital tools like CBT-i Coach and Sleepio offer evidence-based resources you can access from home.
If your symptoms persist for more than two weeks, even with improved sleep routines, it’s essential to consult your healthcare provider for a thorough evaluation.
Preventing Future Sleep and Mental Health Problems
Breaking the cycle of exhaustion and emotional strain that many new mothers face begins with proactive steps to safeguard sleep and mental health.
Creating a Support Network
Start by building a reliable support system. Be specific when asking for help. For example, instead of accepting vague offers, ask a friend to care for your baby from 9:00 a.m. to 12:00 p.m. on Tuesdays so you can rest. Clear requests make it easier for others to provide meaningful assistance.
Professional resources are invaluable as well. The National Maternal Mental Health Hotline (1-833-TLC-MAMA) provides free, 24/7 confidential support in multiple languages, including English and Spanish. Postpartum Support International offers over 50 free virtual support groups led by trained facilitators, with specialized options for military moms or those navigating fertility challenges. Their Peer Mentor Program connects you with volunteers who have personally recovered from perinatal mood disorders, offering guidance and empathy.
At home, formalizing the division of labor is crucial. Work with your partner or support person to create a structured sleep schedule. A clear care plan tailored to your needs ensures that help is targeted and effective.
Custom Postpartum Care Plans
Personalized care plans are another way to prioritize sleep and emotional recovery. These plans treat rest as a non-negotiable part of postpartum care. Whether you need overnight feeding assistance, lactation support to ease breastfeeding challenges, or emotional recovery strategies, a tailored approach addresses your unique needs. For breastfeeding mothers, incorporating pumping into the routine allows a partner or caregiver to handle at least one nighttime feeding, giving you an opportunity for uninterrupted sleep.
Nestling offers customized postpartum care plans that connect you with vetted professionals, such as postpartum doulas, lactation consultants, and infant care specialists. These caregivers provide overnight care, manage feeding routines based on your baby’s developmental stage, and even assist with light household tasks. Their services are designed to reduce both the mental load and physical fatigue that can contribute to depression. Flexible booking options and thorough caregiver verification mean your support system can adapt as your needs evolve throughout the postpartum period.
Conclusion
The connection between sleep deprivation and postpartum depression is one that requires immediate attention. Chronic sleep loss can disrupt vital neurochemical pathways, significantly increasing the risk of postpartum depression.
"Sleep is not optional recovery but a medical necessity." - Phoenix Health Editorial Team
Taking steps to prioritize sleep early is essential - not just for your mental health, but also for your baby’s well-being. Addressing sleep issues promptly can help lessen the impact of postpartum mental health challenges.
If you find that feelings of low mood persist for more than two weeks after improving your sleep, it’s important to seek professional support. As the Phoenix Health Editorial Team reminds us:
"The investment in sleep is a mental health investment."
Your mental well-being is key to both your recovery and your ability to care for your baby. Whether it’s reaching out to friends for help, working with your partner to create a consistent sleep schedule, or enlisting professional overnight caregivers, taking action now can make all the difference. For tailored postpartum support and expert advice on sleep routines, check out Nestling (https://getnestling.com). By prioritizing sleep, you can break the cycle of exhaustion and depression, ensuring you have the strength to care for both yourself and your baby.
FAQs
How can I tell baby blues from postpartum depression?
Baby blues typically show up a few days after giving birth and can last up to two weeks. They often involve mild emotional shifts like mood swings, tearfulness, anxiety, and irritability. Thankfully, these feelings usually fade away without any intervention.
Postpartum depression, on the other hand, is more intense and lasts much longer. It can bring on overwhelming sadness, a sense of hopelessness, trouble bonding with the baby, and noticeable changes in sleep patterns or appetite. Unlike baby blues, postpartum depression often requires professional treatment and emotional support to help with recovery.
What are the fastest ways to get a 4–6 hour sleep block with a newborn?
To help your newborn achieve a 4–6 hour sleep stretch, consistency and attentiveness are key. Start by keeping daytime naps under 2 hours and paying attention to wake windows to avoid overstimulation. Establish a calming bedtime routine to signal that it's time to wind down. Try putting your baby down when they're drowsy but still awake to encourage self-soothing. Keep nighttime interactions quiet and low-key, and respond quickly to their needs to prevent them from becoming overtired. Over time, these practices can support your baby in developing longer sleep periods as they grow.
When should I seek professional help for sleep or mood symptoms?
If you're dealing with persistent sleep or mood issues that interfere with your daily life - especially if you feel hopeless, resentful, or overwhelmed - it’s important to seek professional help. When sleep deprivation extends beyond the usual postpartum fatigue and begins to affect your emotional well-being, your ability to bond with your baby, or your mental health, it’s time to consult a healthcare provider. Left unchecked, ongoing sleep deprivation can increase the risk of postpartum depression, so addressing these concerns early can make a big difference.










