Weaning Tips from Lactation Consultants

Weaning Tips from Lactation Consultants
Weaning doesn’t have to be overwhelming. Here’s a quick summary of practical tips to make the process smoother for you and your baby:
- Go Gradual: Drop one breastfeeding session at a time, starting with the least preferred (usually midday). Wait 3-7 days before eliminating the next session.
- Monitor Breast Health: Watch for signs of discomfort, engorgement, or mastitis. Use cold compresses and express milk sparingly if needed.
- Use “Don’t Offer, Don’t Refuse”: Stop initiating feeds but allow nursing when your child requests it. Redirect with snacks or cuddles over time.
- Introduce New Routines: Replace feeding times with engaging activities like storytelling or walks. Adjust environments to reduce nursing triggers.
- Offer Age-Appropriate Alternatives: Replace breast milk with formula, solid foods, or whole milk, depending on your child’s age.
- Take Care of Yourself: Hormonal changes can bring emotional shifts. Seek support if needed and create new bonding routines with your baby.
- Consult an Expert: Lactation consultants can provide personalized plans and address challenges like discomfort or emotional shifts.
Every family’s journey is unique, and it’s okay to go at your own pace. If challenges arise, don’t hesitate to reach out for professional guidance.
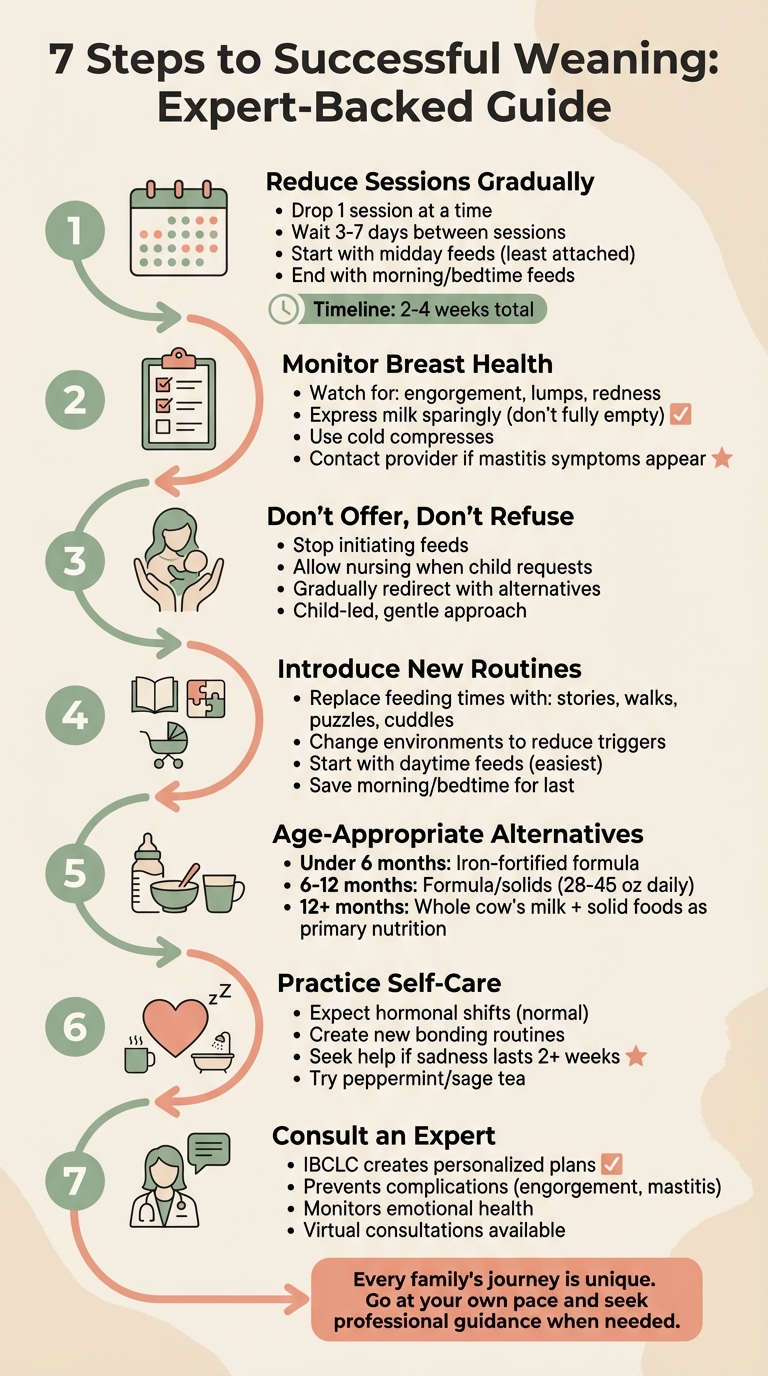
7-Step Weaning Process: Lactation Consultant Guide for Smooth Transition
Weaning: When and How to Gently Wean Your Child!
sbb-itb-9ce2258
1. Reduce Breastfeeding Sessions Gradually
The most effective way to transition is by phasing out one breastfeeding session at a time. This allows both you and your baby to adapt at a comfortable pace. Lactation consultants generally suggest waiting three to seven days before dropping another session, though some recommend extending this to a full week for better adjustment .
Start with the feeding session your baby is least attached to - often the midday feed. Morning and bedtime sessions are usually the last to go since milk production is highest in the morning, and bedtime nursing provides a sense of emotional security. As IBCLC Shoshanna Levine notes:
"The bedtime feed is the last to go because emotions peak at bedtime".
Once you've identified the session to drop, reduce the feeding duration gradually. For instance, if your baby typically nurses for 15 minutes, cut back to 10 minutes first, then continue to decrease over time until the session can be skipped entirely . This gradual reduction engages the Feedback Inhibitor of Lactation (FIL), a natural mechanism that slows milk production when milk remains in the breast .
If you experience discomfort after eliminating a session, express just enough milk to relieve pressure without fully emptying the breast. Fully emptying can signal your body to produce more milk, which may delay the weaning process. Striking this balance helps prevent issues like engorgement, clogged ducts, or mastitis while allowing your milk supply to taper off naturally .
Using this step-by-step method, the weaning process typically takes about two to four weeks . Patience is key, as IBCLC Jennifer Horne explains:
"The faster the weaning process, the more abrupt the shift in hormone levels, and the more likely that you will experience adverse effects".
2. Monitor Your Breast Health and Comfort
As you gradually reduce breastfeeding sessions, keeping an eye on your breast health is crucial to avoid complications. Pay attention to signs like severe fullness, tender lumps, or areas of swelling and redness. These could be early indicators of issues that need attention.
If your breasts feel uncomfortably full, you can use hand expression or a pump for a few minutes to ease the pressure. However, avoid fully emptying your breasts, as this can signal your body to keep producing milk. Persistent symptoms could point to a potential infection.
Mastitis is one condition to be particularly mindful of during weaning. Symptoms include inflamed, red, or hot areas on the breast, ongoing pain, and flu-like symptoms such as chills or fever. If you notice any of these, reach out to a healthcare provider or lactation consultant promptly. Kimberleigh Weiss-Lewit, IBCLC at Boober, emphasizes:
"If you start to feel a plugged duct, pain or mastitis (a breast infection where the tissue is inflamed and you may even develop flu-like symptoms), it is important to remove the milk and reach out to a lactation consultant or your medical provider for support."
To ease discomfort after expressing, cold compresses, ice packs, or chilled cabbage leaves can help reduce swelling and inflammation. A gentle massage during a warm shower can also promote milk flow and prevent clogged ducts. Additionally, wearing a supportive, non-underwire bra can help lower the chances of blocked ducts and infections.
3. Try the Don't Offer, Don't Refuse Method
The "Don't Offer, Don't Refuse" method is a gentle, child-led way to approach weaning. The idea is straightforward: you stop initiating nursing sessions but continue to accommodate your child's requests. Kelly Bonyata, IBCLC, describes it this way:
"Probably the most gentle active approach is 'don't offer-don't refuse'. This method involves not offering to nurse but also not refusing your child's expressed desire to nurse."
This approach helps ease both you and your child into the weaning process at a natural pace.
With this method, your child's interest in nursing gradually decreases, leading to fewer feeding sessions over time. This gradual reduction naturally signals your body to produce less milk. As your child becomes more engaged in activities like playing, eating solid foods, and exploring their environment, the frequency of nursing tends to decline on its own.
You can support this process by minimizing visual cues that may remind your child of nursing. For instance, avoid sitting in your usual nursing spot, such as a favorite chair or corner of the couch. Wearing layered clothing that limits nursing access can also help. Additionally, consider having a non-nursing partner handle routines like wake-up or bedtime to reduce the association with breastfeeding.
This method often takes more time compared to other weaning strategies. During the first week or two, your child may still request nursing. When they do, you can gently redirect them with alternatives like a snack, extra cuddles, or a fun distraction. However, be prepared to nurse if needed. This responsive approach ensures your child feels secure and supported throughout the transition.
4. Introduce New Activities and Routines
Shifting your child's focus away from breastfeeding can often be achieved by introducing new routines, especially during usual nursing times. Daytime feedings tend to be the easiest to replace since children are naturally more active and easily distracted during these hours. Midday sessions, in particular, are often the first to go, as they’re typically the least emotionally significant for your child.
To ease the transition, try offering engaging alternatives before your child even asks to nurse. If you know a usual feeding time is approaching, redirect their attention with activities like puzzles, art projects, storytime, or even a walk. Heidi Szugye, DO, IBCLC, Medical Director of Cleveland Clinic's Breastfeeding Medicine Clinic & Center, explains:
"The change in routine will make it less likely your baby will feel the natural triggers involved with breastfeeding".
Changing the environment can also help reinforce new habits. For example, if your child tends to nurse more at home, plan outings during those times - visit a park, take a walk, or arrange a playdate. Trina Goodwin, Certified Lactation Educator Counselor, suggests:
"If the baby usually nurses upon waking, try getting up before your baby and have your partner or someone else do the morning routine".
This strategy helps break the link between waking up and nursing.
To maintain a sense of comfort, offer physical closeness through cuddles, rocking, or extra snuggles. For older children, introducing a "lovey" - a special blanket or stuffed animal - can provide reassurance during this transition. Additionally, offering a healthy snack or a cup of water just before the usual nursing time can help curb hunger before they ask to nurse.
Keep in mind that morning and bedtime feedings are often the most challenging to replace. These sessions are deeply tied to comfort and routine, so it’s best to phase them out gradually, starting with the easier daytime feedings. Allow your child time to adjust to each new routine before moving on to the next step.
5. Replace Feedings with Age-Appropriate Options
As you introduce new routines to shift away from nursing, it’s important to align feeding alternatives with your child’s developmental needs. Choose substitutes that suit their age and stage of growth.
For babies under 6 months, replace breastfeeding with iron-fortified infant formula. If you’re planning early weaning, consider introducing a bottle of expressed breast milk around 6 weeks.
Between 6 and 12 months, transition to formula or expressed breast milk served in a bottle or cup. At this stage, you’ll also start introducing solid foods. Begin with 1 to 2 tablespoons of iron-fortified rice cereal mixed with breast milk or formula. To monitor for allergies, introduce only one new food each week. During this period, babies typically need 28 to 45 ounces of breast milk or formula daily. If your baby is over 9 months old, you can bypass the bottle altogether and go straight to a sippy or straw cup.
At 12 months and beyond, whole cow’s milk can take the place of breast milk as their main drink. Solid foods should now become their primary source of nutrition, with cow’s milk serving as a supplement. Keep in mind, cow’s milk is not suitable for children under 1 year old.
As noted earlier, start by dropping the midday feeding first, leaving morning and bedtime feedings for later. For children older than 12 months, gradually move the last milk feeding to earlier in the evening to help separate it from their bedtime routine.
"All other foods or beverages are not the nutritional powerhouse that breast milk is and should be fed after breast milk, complimentary to it, not in place of it".
This approach can help set realistic expectations as you navigate the weaning process.
6. Practice Self-Care During the Transition
Weaning isn’t just a physical process - it’s an emotional one too. When breastfeeding comes to an end, your body experiences a drop in bonding and calming hormones, which can trigger feelings similar to the baby blues. You might notice emotions like sadness, anxiety, irritability, or even a sense of loss or frustration. These feelings are completely normal.
"You are not too sensitive. Weaning is a real goodbye, and goodbyes stir things up." - Motherly
The upside? These mood changes are usually temporary. But if you find that sadness or intrusive thoughts linger for more than two weeks, it’s important to reach out to a healthcare provider. Persistent feelings could be a sign of post-weaning depression, which may need professional attention.
While navigating these emotional shifts, don’t forget to care for your body too. To ease physical discomfort, you can revisit earlier tips like using cold compresses, brief expression techniques, or wearing supportive bras. Drinking peppermint or sage tea throughout the day might also help reduce your milk supply naturally.
On the emotional side, creating new bonding routines can help both you and your baby adjust. For example, you could replace nursing sessions with extra cuddles, reading a favorite book, or enjoying skin-to-skin time. Writing down your reasons for weaning can also be a helpful reminder when feelings of guilt arise. Some parents even find comfort in marking the transition with a small ritual, like taking a special photo or writing a letter to their baby. And don’t underestimate the power of talking - sharing your feelings with a partner, friend, or counselor can provide much-needed support.
"Relief and sadness can sit in the same lap. You are allowed to feel both." - Motherly
7. Get Help from a Lactation Consultant
You don’t have to navigate weaning on your own. Partnering with an International Board Certified Lactation Consultant (IBCLC) can give you a step-by-step plan tailored to your family’s unique needs. These professionals assess your baby’s readiness for weaning alongside your physical and emotional state, helping to create a timeline that works for both of you.
An IBCLC can also help you sidestep challenges like painful engorgement or mastitis by crafting a gradual pump-to-comfort plan. This approach gently signals your body to slow down milk production, reducing the risk of discomfort. Beyond the physical aspects, they’ll keep an eye out for signs of post-weaning depression and suggest ways to maintain a strong bond with your baby through non-nursing activities. As IBCLC Jennifer Horne puts it:
"An IBCLC can help answer questions about the process and create a care plan that works for both you and your baby."
Adrienne Koznek, another IBCLC, highlights the importance of support during this time:
"With proper guidance and support, it can be done in a way that ensures good physical and emotional health of both the breastfeeding parent and the child."
Weaning usually takes about 2–4 weeks, though the timeline can vary. The key is to seek help early - before issues like clogged ducts or feelings of overwhelm set in. Virtual consultations have made it even easier to access expert guidance, letting you connect with a lactation consultant from the comfort of your own home.
For families looking for personalized support, Nestling offers access to vetted lactation consultants who specialize in creating care plans that address both physical and emotional transitions. With thorough verification and flexible booking options, Nestling ensures you can find the right expert to guide you through this important stage of your journey.
Conclusion
Weaning doesn’t have to feel like an uphill battle if you take it step by step. The approaches discussed here - like the "don't offer, don't refuse" method or swapping nursing sessions for other bonding activities - can make the process smoother for both you and your child. Taking a gradual path not only reduces the risk of complications but also gives your body time to adjust.
Every family’s journey is different. What works perfectly for one may not align with another’s routine or emotional dynamics. You might opt for partial weaning, holding onto a morning or bedtime session for some extra closeness, or slowly transitioning away from all feedings. And it’s okay to pause if your child is teething, feeling unwell, or going through a developmental leap. Tailor these strategies to fit your unique situation.
Dr. Heidi Szugye from Cleveland Clinic emphasizes this beautifully:
"The decision to wean, and the reasons behind weaning, are different for every family."
Trust your instincts as you navigate this transition. If you feel unsure or face challenges, reaching out for professional support can make a big difference. Lactation consultants can create customized care plans to guide you through the physical and emotional aspects of weaning, helping you avoid potential issues.
For extra support, Nestling offers access to vetted IBCLC experts through flexible virtual consultations. Whether you’re just starting to think about weaning or are already in the midst of it, expert advice can help you feel confident and prepared as you implement these strategies.
FAQs
How do I wean without getting mastitis?
To reduce the risk of mastitis while weaning, it's important to take things slow. Gradually decrease how often and how long you nurse or pump, and extend the time between sessions. If you notice engorgement or discomfort, try gentle expression or apply cold compresses for relief. Be careful not to fully empty your breasts, as this can signal your body to produce more milk. By easing into the process, you can help your body adjust while minimizing the chances of clogged ducts and infection.
What if my baby only wants to nurse at bedtime?
If your baby tends to nurse at bedtime, consider easing the transition by slowly introducing new calming bedtime routines. You could try reading a book, singing a lullaby, or offering cuddles to create a comforting environment. Gradually shortening nursing sessions can also help your baby adjust and reduce their reliance on breastfeeding for sleep. The process takes time, so stay patient and consistent as your baby adapts.
When should I contact a lactation consultant for weaning help?
If you're looking for a gradual and personalized approach to weaning, connecting with a lactation consultant can be incredibly helpful. They can guide you through the process, addressing any challenges - like emotional hurdles or specific concerns - and help make the transition easier for both you and your baby.










