5 Steps To Safely Progress Post-C-Section Workouts

5 Steps To Safely Progress Post-C-Section Workouts
Recovering from a C-section takes time, patience, and the right approach to exercise. Here's a quick guide to help you safely regain strength and rebuild your core after surgery:
- Start with Breathing and Core Activation: Begin gentle diaphragmatic breathing and transverse abdominis contractions to reconnect with your core muscles.
- Introduce Low-Impact Strengthening: Around 4–6 weeks postpartum, try exercises like glute bridges and ball squeezes to strengthen your pelvic floor and core.
- Add Functional Movements and Walking: Incorporate everyday movement patterns and gradually increase your walking duration to improve stability and endurance.
- Rebuild Rotational Core Strength: After 6–12 weeks, include rotational exercises like opposite knee presses and Pallof presses to restore functional strength.
- Transition to Full-Body Workouts: By 12 weeks, progress to bodyweight exercises, light cardio, and eventually resistance training, but only if you're pain-free and cleared by your doctor.
Key Reminder: Always listen to your body. Stop immediately if you experience sharp pain, pelvic pressure, urinary leakage, abdominal bulging, or discomfort near your incision. Consult a healthcare provider or postnatal care specialist for personalized guidance.
This step-by-step plan ensures a gradual, safe recovery while helping you rebuild strength and confidence over time.
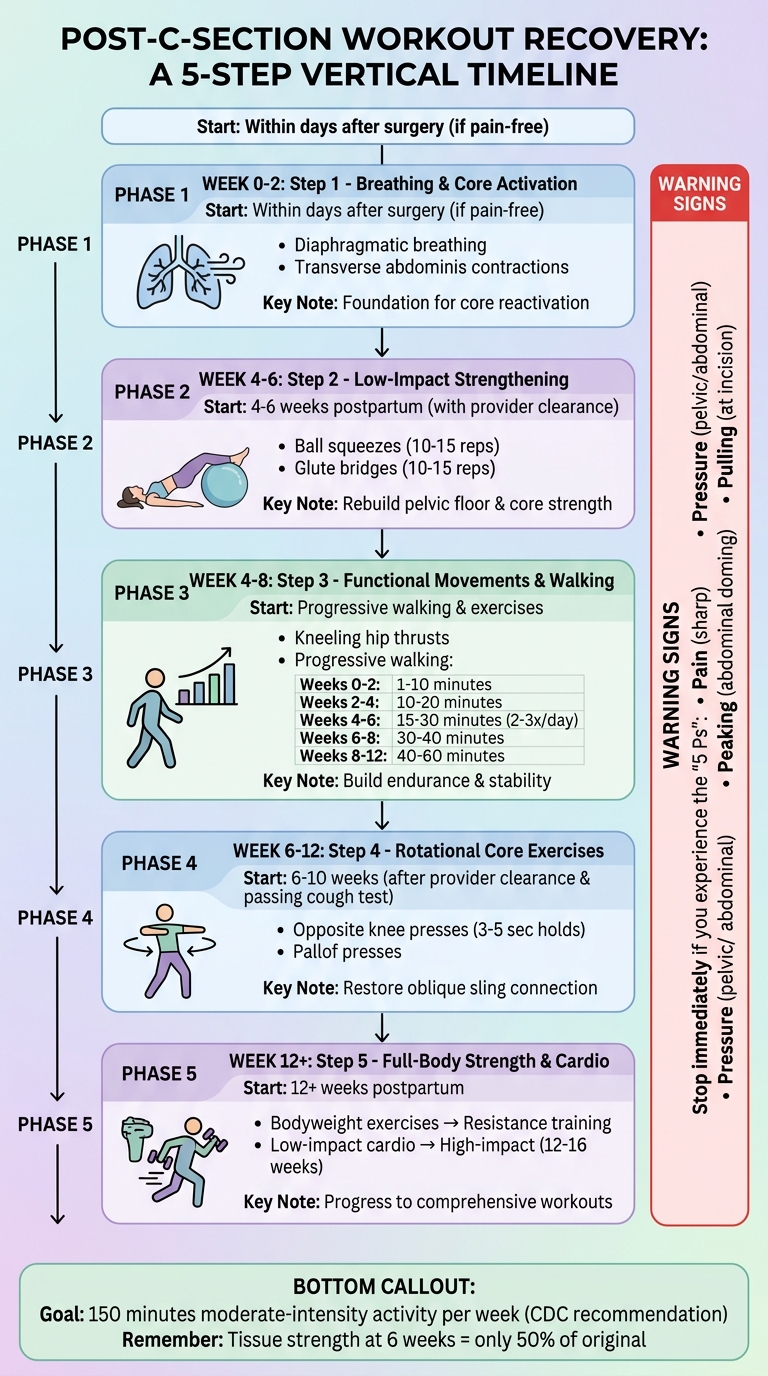
5-Step Post-C-Section Workout Recovery Timeline: Weeks 0-12+
C-Section Recovery Plan: Workout #2 - heal and strengthen your body post C-section, postpartum
sbb-itb-9ce2258
Step 1: Begin with Breathing Exercises and Core Activation
Following a cesarean delivery, your diaphragm, pelvic floor, abdominal muscles, and back need to work together again. Breathing exercises are a great way to retrain this coordination, which is essential for stability in daily activities. Wendy Powell, Founder and CEO of MUTU System, emphasizes:
"Your core is the foundation of your body!"
Pregnancy and surgery can disrupt the neural connection to your abdominal muscles, so reactivating your core early is key. Engaging these muscles properly can relieve pressure on your incision, reduce back pain, and improve issues like pelvic discomfort or urinary incontinence. These gentle exercises also increase blood flow, which helps with tissue recovery and scar healing.
How to Practice Diaphragmatic Breathing
Diaphragmatic breathing can typically be started within a few days after surgery, as long as it’s pain-free. To try it, lie on your back with your knees bent and feet flat. Place one hand on your ribcage and the other on your belly. Slowly inhale through your nose for about 4 seconds, allowing your ribs to expand and your belly to rise. Then exhale through pursed lips for 4 seconds, feeling your belly fall and your ribcage relax. If your incision is tender, gently support it with a pillow.
This breathing technique forms the base for activating your core effectively.
Performing Transverse Abdominis Contractions
Once you’re comfortable with diaphragmatic breathing, you can add gentle abdominal draw-ins. While lying on your back with knees bent, take a breath in to prepare. As you exhale, slowly draw your lower belly toward your spine, as if you’re zipping up a pair of jeans. To add more benefit, include a light pelvic floor lift (a Kegel exercise) at the same time, keeping your effort at about 30% to 40% of your maximum. Start with 10 repetitions and gradually work up to 2–3 sets as you gain strength. Be cautious and stop immediately if you notice bulging along the midline of your abdomen, sharp pain at the incision, or any pelvic pressure.
Step 2: Add Low-Impact Strengthening Exercises
Once you've activated your core, it's time to move on to gentle strengthening exercises. These exercises are designed to help your pelvic floor and core regain their strength and stability, which may have been affected by pregnancy or surgery. Prenatal yoga instructor Laura Staton emphasizes the importance of this step:
"Exercise can help your pelvic floor and core bounce back, and it lets you take control of your body."
If your healthcare provider gives you the green light, you can start these low-impact exercises around 4–6 weeks after your C-section. These movements are carefully chosen to re-engage your muscles and improve blood flow to the pelvic area without putting undue stress on your healing incision. Strengthening your glutes and inner thighs also plays a key role in stabilizing your hips and pelvis, which can help address the postural changes brought on by pregnancy. By building on the foundation of core activation, these exercises set the stage for more advanced, full-body workouts down the line.
Ball Squeezes for Inner Thigh and Core
Ball squeezes are a great way to engage your inner thighs, pelvic floor, and deep core muscles all at once. Here’s how to do them:
- Sit upright or lie on your back with your knees bent and feet flat on the floor.
- Place a yoga block, soft pillow, or soccer ball between your knees.
- Inhale deeply to prepare, then exhale as you squeeze the object between your knees. At the same time, gently pull your lower abdomen toward your spine and lift your pelvic floor.
Start with 1 set of 10–15 repetitions. As your strength improves, you can work up to 2–3 sets.
Glute Bridges for Hip Stability
Glute bridges are excellent for targeting muscles that may have weakened during pregnancy. To perform them:
- Lie on your back with your knees bent and feet flat on the floor, about hip-width apart.
- Inhale, then exhale as you press through your heels to lift your hips. Your body should form a straight line from your shoulders to your knees.
- At the top, squeeze your glutes and engage your lower abdomen and pelvic floor. Keep your upper back and shoulders grounded, and avoid lifting your hips too high to prevent straining your lower back.
Begin with 1 set of 10–15 repetitions. Over time, increase to 2–3 sets and consider holding the top position for up to 5 seconds.
Important: Stop immediately if you notice urinary leakage, pelvic pressure, sharp pain, or abdominal doming. If you feel tightness or pulling around your C-section scar during any movement, reduce your range of motion or wait a bit longer before attempting these exercises again.
Step 3: Include Functional Movements and Walking
Once you've established a foundation with low-impact strength exercises, it's time to incorporate movements that mirror everyday tasks. These functional movements are designed to engage your core and prepare your body for real-life demands - like lifting your baby. By training your body to exhale and activate the deep core during movement, you help protect your pelvic floor and reduce the risk of injuries. These exercises naturally connect to the way your body moves in daily life, making them incredibly practical.
Kneeling Hip Thrusts for Hip and Core Stability
Kneeling hip thrusts are excellent for targeting the hips and glutes while helping your core learn to stabilize during motion. They can also counteract the rounded shoulders that often develop from breastfeeding. Here's how to do them:
- Kneel on a soft surface with your knees hip-width apart. Place your hands on your hips or cross them over your chest.
- Take a deep breath in to prepare. As you exhale, press your hips forward and engage your glutes.
- Keep your ribs aligned with your pelvis and maintain a neutral lower back.
- Slowly return to the starting position. Progress at your own pace as your strength improves.
Pay attention to your body. Stop immediately if you notice any of the "5 Ps": Pain, Pressure (in the pelvic or abdominal area), Pee (leakage), Peaking (doming at the midline), or Pulling at your incision site.
Developing a Walking Routine
Walking is a great recovery tool that reintroduces upright movement, gently engages the pelvic floor, and reconnects your core with your breathing mechanics. As you build strength and coordination through functional exercises, you'll be better prepared for walking routines. Start small and increase your walks over time:
- Weeks 0–2: Begin with 1–10 minute walks indoors.
- Weeks 2–4: Progress to 10–20 minute walks on flat terrain.
- Weeks 4–6: Aim for 15–30 minute walks, 2–3 times a day.
- Weeks 6–8: Extend to 30–40 minute sessions, adding gentle inclines.
- Weeks 8–12: Work up to 40–60 minutes, and consider fitness walking or walk-to-jog intervals.
A few precautions to keep in mind: During the first few weeks, avoid pushing a stroller or carrying heavy loads while walking. If you feel any pulling at your incision, an abdominal belt or belly band can provide extra support. Focus on standing tall rather than slouching to help your incision heal properly and to prevent adhesions. If you notice pelvic pressure, urinary leakage, abdominal doming, or increased postpartum bleeding, stop walking immediately and consult your healthcare provider.
Step 4: Add Rotational Core Exercises
As you move beyond basic core activation and low-impact movements, it’s time to rebuild rotational strength. Once your foundational core and functional strength are in place, you can start incorporating rotational exercises. These are especially important because a cesarean delivery involves cutting through the anterior oblique sling - a muscle chain that runs from your chest, across the obliques and pubic symphysis, to the opposite inner thigh. Reintroducing rotational exercises helps restore the neuromuscular connection in this chain, which is key for functional rotational movements in daily life.
"During a cesarean birth, the anterior oblique sling is cut which can affect our core connection. This sling supports rotational movements to the front (think opposite shoulder to knee)." - Gina Conley, MS, MamasteFit
Before starting, ensure you have clearance from your healthcare provider, which is typically given between 6 to 10 weeks postpartum. You should also pass the "cough test": when you cough, your abdominal wall should draw inward and remain flat. If it bulges outward, your core may not yet be ready for increased pressure. Most experts recommend waiting until around 12 weeks post-C-section before introducing resistance-based rotational work, allowing time for the fascia to heal adequately.
Opposite Knee Presses for Core Stability
This simple yet effective exercise helps reconnect your obliques and trains your core to stabilize against resistance. Start by lying on your back with your knees bent and feet flat on the floor. Take a deep breath to prepare. As you exhale, gently engage your lower belly and press one hand against the opposite knee. Hold this isometric press for 3–5 seconds, ensuring your belly stays flat or slightly drawn in - avoid any bulging upward. Release and repeat on the other side.
Prioritize quality over quantity. Move slowly and with control, focusing on keeping your transverse abdominis engaged throughout the exercise. If you notice any doming at the midline, pelvic pressure, or discomfort near your incision, stop immediately and reduce the intensity. Once you’ve mastered this, you can progress to exercises that improve anti-rotational control.
Pallof Presses for Anti-Rotational Strength
The Pallof press is an excellent exercise for building anti-rotational strength, which trains your core to stabilize your spine and pelvis against external forces. This skill is essential for everyday movements. You’ll need a light resistance band anchored at chest height. Stand or kneel perpendicular to the anchor point, holding the band at your chest with both hands. Keep your feet hip-width apart for stability.
Inhale to prepare, then exhale as you press the band straight out in front of you, resisting the pull to rotate toward the anchor point. Hold this position for 3–5 seconds while maintaining steady breathing, then slowly bring your hands back to your chest. You can perform this exercise in various positions - lying on your back, seated, or half-kneeling - to find the variation that best suits your recovery stage.
Keep your ribs aligned over your pelvis to properly engage your deep core muscles. Start with very light resistance and only increase it as your strength improves. Make sure your movements are controlled, avoiding momentum or compensatory actions.
Step 5: Progress to Full-Body Strength and Cardio
Around 12 weeks postpartum, many women are ready to transition to full-body routines, but it’s important to remember that recovery timelines can vary. Working with postnatal care specialists can help you navigate these individual differences safely. This stage builds on earlier core and rotational work, preparing you for a more comprehensive workout plan.
"The focus should be on rebuilding your core and pelvic floor muscles during the first 12 weeks after birth before returning to higher impact activity such as running, weightlifting or high-intensity interval training." - Sara Reardon, PT, DPT, WCS
As you move forward, listen to your body closely. Stop immediately if you notice sharp pelvic pain, increased vaginal bleeding, bulging at your abdominal wall, urinary leakage, pelvic pressure, or discomfort at your incision site.
Exercise Progressions from Beginner to Advanced
Start with bodyweight exercises to build a strong foundation before adding resistance. For example:
- Squats: Begin around 6 weeks postpartum using just your body weight. Once you’re comfortable, add a resistance band around your knees or light dumbbells to increase intensity.
- Bridges: Safe to start between 4–6 weeks postpartum with your feet flat on the floor. To make them more challenging, use a resistance band for added glute engagement.
- Push-ups: Wall push-ups are a gentle way to build upper body strength starting at 4 weeks postpartum. Progress to incline push-ups and, eventually, floor push-ups as your core stabilizes.
Wall sits are another great option for strengthening your legs and engaging your core. These can be safely introduced at 6 weeks postpartum. Keep in mind that at this stage, your abdominal tissue is still regaining strength - it’s only about 50% of its original tensile strength at six weeks. To protect your pelvic floor and any surgical sites, exhale during the exertion phase of each movement.
| Exercise | Start Time | Beginner Option | Advanced Progression |
|---|---|---|---|
| Squats | 6 Weeks | Bodyweight only | Add resistance bands or light dumbbells |
| Bridges | 4–6 Weeks | Feet flat on floor | Use a resistance band around knees |
| Push-ups | 4 Weeks | Wall push-ups | Incline or floor push-ups |
Adding Cardio and Strength Training Safely
Once you’ve built a solid base of strength, gradually incorporate cardio. Walking is an excellent starting point - begin with short 5–10 minute walks and work up to 30–45 minutes by week 6. Low-impact options like stationary cycling or using an elliptical machine can also be introduced. If you’re considering swimming, wait until 4–6 weeks postpartum, ensuring all bleeding has stopped and your incision is fully healed to avoid infection risks.
High-impact activities such as running, jumping, or high-intensity interval training should typically wait until 12–16 weeks postpartum. These should only be attempted if you’re pain-free, have strong core stability, and can maintain proper form. Before advancing, check that your midline remains stable during movement. To monitor your effort level, use the "talk test" - you should be able to hold a conversation without gasping for air. The CDC recommends gradually increasing to 150 minutes of moderate-intensity aerobic activity per week.
"Too often, women push for results with high-impact activity too soon. Respect the process. Healing matters just as much as hustle." - Carmen Bott, Fitness Expert
Getting Expert Support for Your Recovery
When transitioning to full-body workouts, having expert support can make all the difference in ensuring your recovery is both safe and effective. While your 6-week postpartum checkup confirms that external incisions have healed, a visit to a pelvic floor physical therapist offers a deeper look at your recovery. These specialists evaluate pelvic floor muscle function, C-section scar tissue mobility, and overall movement patterns - because the pelvic floor doesn't operate in isolation.
This type of assessment is especially important since recovery from a C-section often takes longer than many people expect. While the initial healing phase lasts around 6–8 weeks, scar tissue continues to mend for over a year. Just as each exercise builds on the previous one, expert evaluations ensure your recovery plan is tailored to your specific needs. A pelvic floor physical therapist can teach you scar massage techniques (usually introduced after 6 weeks) to help improve the appearance and texture of your incision. These techniques can also help prevent complications like urinary incontinence, pelvic organ prolapse, and chronic pelvic pain.
If you notice symptoms such as urinary leakage, a feeling of pelvic heaviness, sharp pain, or abdominal bulging, it’s important to consult a specialist right away.
Nestling connects you with trusted postpartum care experts, including postpartum doulas and lactation consultants, to provide personalized support for both your newborn care and your recovery journey.
Conclusion
Recovering from a C-section requires patience and respecting your body's natural healing process. Start with diaphragmatic breathing and gentle pelvic floor activation, then gradually move to low-impact exercises like glute bridges and ball squeezes. As you progress, include functional movements and walking, followed by rotational core exercises, before transitioning back to full-body strength training and cardio. This structured approach helps protect your incision and rebuilds core stability step by step.
"Think of early postnatal fitness as rehabilitation rather than traditional exercise. You are teaching your body how to move well again from the inside out." - Parenting.ra6.org
If you notice sharp pain near your incision, experience urinary leakage, feel pelvic heaviness, or see abdominal bulging, stop immediately and consult your healthcare provider.
While your six-week checkup may confirm external healing, remember that internal tissues often require more time to recover. The CDC advises aiming for 150 minutes of moderate-intensity activity per week, which you can break into manageable sessions that suit your schedule and energy levels. Focus on movement quality and use the talk test to maintain a sustainable intensity. These recommendations highlight the importance of pacing yourself as you rebuild strength over time.
"The key is to be patient. Avoid pressuring yourself to 'bounce back.' Instead, focus on moving your body because it helps you feel better and fuels the energy you need." - Pampers
Take it slow, listen to your body, and build strength at a pace that works for you. For additional support, consider reaching out to trusted postpartum professionals through Nestling to guide you on this journey.
FAQs
How do I know I’m ready to progress to the next step?
Once your healing has progressed and you have your doctor’s approval, you can start incorporating more advanced postpartum exercises. Early on, gentle activities like deep breathing and short walks are great for easing into movement, often beginning shortly after surgery. However, more intense workouts are typically delayed until about six weeks after delivery.
Pay attention to your body. Signs that you may be ready to step up your exercise routine include minimal pain, no heavy bleeding, and feeling comfortable during movement. To ensure you’re on the right track, consult your healthcare provider or a pelvic floor therapist for personalized advice.
What are the biggest exercise mistakes to avoid after a C-section?
Starting high-impact exercises too early - like sit-ups, planks, or jumping - can put unnecessary strain on your incision and core. It’s important to wait until your healthcare provider gives you the green light, which usually happens around 6 weeks postpartum. Instead, focus on gentle activities to ease back into movement. Deep breathing, ankle pumps, and short walks are great starting points as your body recovers. Gradually increase intensity, but always stick to exercises that promote healing without overloading your core.
When should I see a pelvic floor physical therapist?
It's a good idea to visit a pelvic floor physical therapist about six weeks after giving birth, even if your OB or midwife has already given you the green light. These specialists can evaluate your pelvic muscles, check any scar tissue, and analyze your movement patterns. This helps ensure you're safely easing back into postpartum workouts. They can also offer tailored advice on how to reintroduce pelvic floor and core exercises, particularly after a C-section.