How To Build Emotional Resilience Postpartum

How To Build Emotional Resilience Postpartum
The postpartum period is challenging, but building emotional resilience can make it easier to manage. Here's how you can handle stress, recover emotionally, and create a supportive environment during this time:
- Self-Compassion Matters: Be kind to yourself. Set realistic expectations, use positive self-talk, and reframe negative thoughts to stay balanced.
- Mindfulness Helps: Breathing exercises, sensory grounding, and mindful activities like walking or feeding can keep you present and calm.
- Support Systems Are Key: Lean on family, friends, postpartum groups, or postpartum specialists for emotional and practical help.
- Prioritize Sleep and Self-Care: Focus on rest, gentle physical activity, and a balanced diet to boost your energy and mood.
- Know When to Seek Help: If feelings of sadness or anxiety persist, reach out to a therapist or healthcare provider for support.
Resilience isn’t about avoiding tough emotions but learning to manage them effectively. By combining these strategies, you can navigate postpartum life with more confidence and ease.
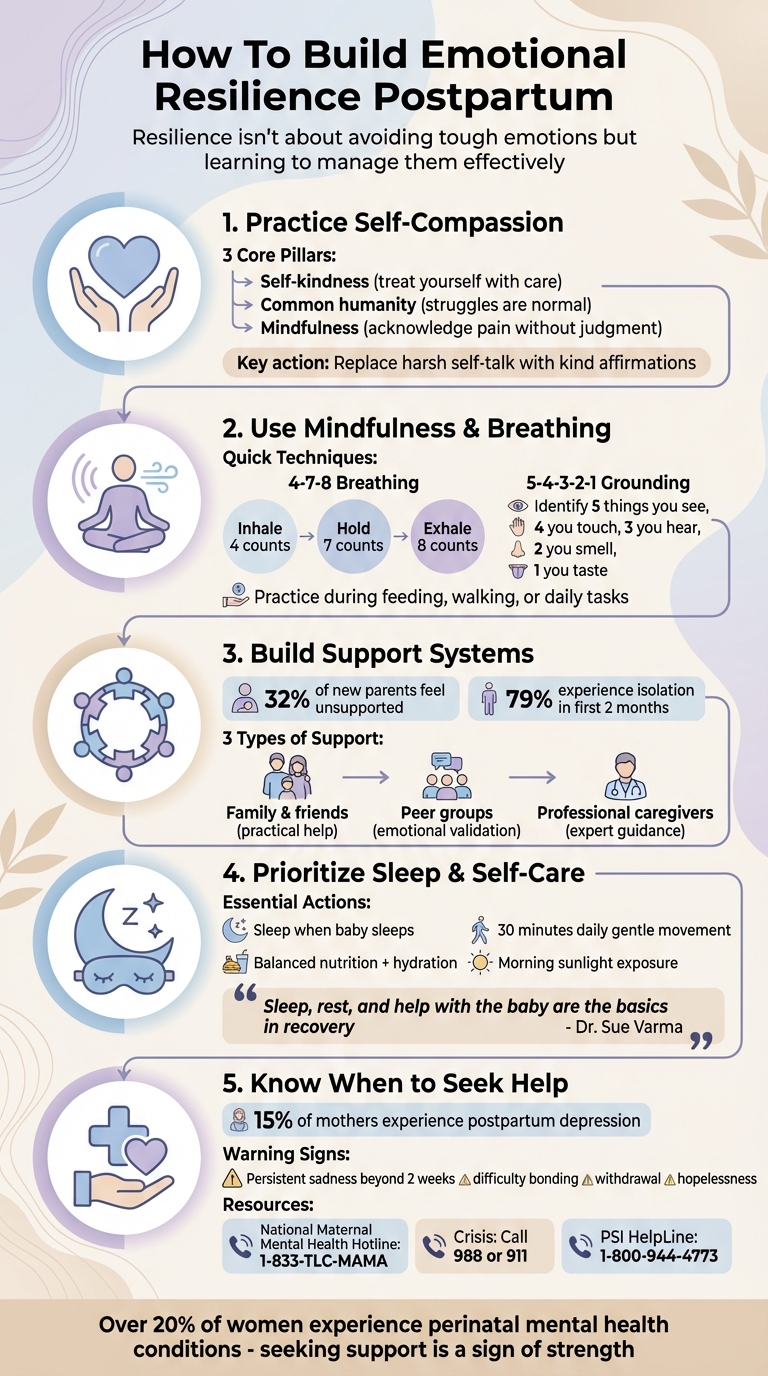
5 Essential Strategies to Build Emotional Resilience Postpartum
Perinatal Mental Health: Tips for Pregnancy & Postpartum Wellness
sbb-itb-9ce2258
Practice Self-Compassion
Navigating the early days of parenthood can bring a mix of emotions - guilt, self-doubt, and even a sense of being overwhelmed. Practicing self-compassion can be a game-changer during this time. As psychotherapist Sarah Duran reminds us:
The postpartum period is not about bouncing back; it's about recovering and adapting.
Self-compassion works by calming your inner alarm system and activating self-soothing mechanisms, releasing oxytocin - the hormone that helps you feel more at ease. It’s not about striving for perfection. Instead, it’s about showing yourself the same kindness you’d offer a close friend going through a tough time. Studies reveal that parents who practice self-compassion tend to maintain a steady sense of self-worth, regardless of daily ups and downs.
Kristin Neff, a leading voice in self-compassion research, beautifully explains:
Self-compassion provides an island of calm, a refuge from the stormy seas of endless positive and negative self-judgment.
This practice is built on three pillars: self-kindness (treating yourself with care instead of criticism), common humanity (understanding that struggles are part of being human), and mindfulness (acknowledging pain without blowing it out of proportion). Let’s explore how these principles can be applied in everyday life: creating a self-care routine for new moms that includes setting realistic expectations, speaking kindly to yourself, and reframing negative thoughts.
Set Realistic Expectations
The societal pressure to "bounce back" after childbirth can be a heavy burden, leading to feelings of inadequacy. Instead, allow yourself to lower the bar during those early weeks. An untidy home, a chaotic routine, or relying on takeout meals doesn’t mean you’re failing - it means you’re focusing on healing and adapting.
Shifting from a perfectionist mindset to one of progress can be liberating. Acknowledge that adjusting to parenthood is a monumental life shift, and feeling challenged is completely normal. By setting practical expectations, you create room for growth and self-discovery without the weight of harsh self-judgment. This approach builds a foundation for resilience and recovery.
Use Kind Self-Talk
Pay attention to your inner voice. When critical thoughts crop up, pause and ask yourself, "Would I speak this way to a friend?". If the answer is no, replace those harsh words with the compassion you’d offer someone you care about.
Here are a few affirmations to consider:
- "I am doing my best, and that is enough"
- "It’s okay to make mistakes; I’m not perfect"
- "May I offer myself kindness as I care for my baby"
Even small physical gestures can reinforce this practice. Placing a hand over your heart or giving yourself a gentle hug can release oxytocin and ease stress. Another helpful tool is the "Self-Compassion Break." Start by acknowledging the difficulty ("This is hard right now"), remind yourself that others face similar struggles, and offer yourself words of kindness.
Reframe Negative Thoughts
Our minds naturally lean toward negativity, but reframing your thoughts can help shift your focus to a more balanced perspective. Instead of labeling yourself harshly, try restating the situation in neutral terms.
For instance, swap "I’m a failure for not breastfeeding" with "Breastfeeding is challenging today, and I’m exploring other options". Or replace "I’m a bad mom" with "I’m feeling overwhelmed right now". This small shift in language can reduce the emotional intensity of tough moments.
Use Mindfulness and Breathing Practices
Mindfulness can be a lifeline when you're navigating the challenges of feeding, sleep, and parenting. Licensed holistic psychotherapist Kim Burris explains it best:
Mindfulness simply means focusing your attention and awareness on the present moment.
The beauty of mindfulness is its flexibility - you don’t need a quiet room or a special setup. You can practice it while soothing your baby, changing a diaper, or even during those long, sleepless nights. The goal isn’t to push away tough emotions but to recognize them without letting them take over.
Here’s how you can weave mindfulness into your daily postpartum routine.
Try Breathing Exercises for Calm
Breathing exercises are a simple yet powerful way to center yourself, even while holding your baby. One effective technique is the 4-7-8 breathing method: inhale through your nose for 4 counts, hold your breath for 7 counts, and exhale slowly through your mouth for 8 counts.
Another option is controlled rhythmic breathing. Breathe in slowly through your nose for three seconds, then exhale through your mouth for three seconds. These exercises take just a minute but can help you regain a sense of calm when things feel overwhelming.
Use Sensory Grounding Techniques
If breathing exercises don’t quite do the trick, grounding techniques can provide additional support.
A quick and practical method is the 5-4-3-2-1 technique. For example, during a diaper change or bath time, look around and identify:
- Five things you can see
- Four things you can touch
- Three things you can hear
- Two things you can smell
- One thing you can taste
This exercise shifts your focus to your surroundings, breaking the cycle of anxious thoughts. Dr. Edith Gettes, Medical Director of the UNC Women's Mood Disorder Clinic, notes:
Engaging senses slows down the buzz of the mind.
If you’re feeling especially disconnected or “spaced out,” try pressing your heels firmly into the floor. This simple action can help ground you and bring you back to the present moment.
Practice Mindful Walking and Feeding
Feeding your baby - whether by breastfeeding or bottle-feeding - is a natural time to practice mindfulness. Pay attention to the warmth of your baby’s body, the sound of their swallowing, and the gentle rhythm of their breathing. When your thoughts wander, gently guide them back to the moment, without judgment.
Mindful walking can also be a grounding activity. While taking a stroll with your baby, focus on the rhythm of your steps and the sensation of the air on your skin. If thoughts about chores or emails creep in, acknowledge them and let them drift away. Each step becomes an opportunity to build emotional strength.
Incorporating these mindful habits into your routine can help you stay grounded and resilient, complementing the self-compassion and support strategies discussed earlier.
Build and Rely on Support Systems
Having a strong support system is essential for postpartum recovery. It’s not just about managing the physical demands of caring for a newborn - it’s also about safeguarding your emotional well-being. Research highlights that 32% of new parents feel unsupported, and 79% experience isolation in the first two months after giving birth. Establishing a dependable network of support before and after your baby arrives can help you navigate this challenging period with greater ease.
The best support systems combine three key elements: informal support from family and friends who can help with everyday tasks, peer support from other parents who understand your experience, and professional care from experts trained to provide guidance. Dr. Angelica Glover, an ob-gyn, stresses the importance of planning ahead:
The time to talk about postpartum support is before your baby is born... This way we map out the postpartum support network in advance.
Let’s explore how these types of support can make a difference.
Connect with Family and Friends
Your loved ones can be a lifeline, but it’s important to communicate clearly about what you need. Instead of general requests, ask for specific help, such as “Can you pick up groceries on Tuesday?” or “Could you watch the baby for two hours so I can rest?” The U.S. Department of Health & Human Services advises:
Be specific. Do you need a ride to appointments, help with groceries or childcare, or someone to listen?
Consider creating a household manual during your third trimester. This document can include instructions for laundry, meal prep, and baby care routines, making it easier for others to step in without needing constant direction. It’s also a good idea to share any warning signs - like feeling unusually fatigued or out of breath - with trusted individuals, so they’ll know when you might need extra support.
Join Postpartum Support Groups
While help from family is invaluable, connecting with other parents who are in the same boat can reduce feelings of loneliness and provide emotional validation. Research backs this up: A study of 100 first-time mothers found that peer telephone support lowered depression scores from 13.29 to 10.25 over eight weeks.
Postpartum Support International (PSI) offers over 50 free weekly Zoom groups where parents can connect and share experiences. You can find groups tailored to your specific needs, whether you’re a parent of multiples, a military mom, or looking for culturally aligned support. Prefer phone support? The PSI HelpLine (1-800-944-4773) and the National Maternal Mental Health Hotline (1-833-TLC-MAMA) are available for confidential assistance.
Work with Professional Caregivers
Sometimes, you need expert help to navigate the complexities of postpartum life. Postpartum doulas and lactation consultants offer three types of essential support: emotional (providing reassurance and empathy), instrumental (helping with practical tasks like childcare and household chores), and informational (guidance on feeding, sleep routines, and newborn care).
Ali Sugarman, a postpartum doula, describes their role:
Postpartum doulas also help with this aspect - they are a non-judgmental support system here to help you cope with the emotional rollercoaster of parenthood.
If you’re looking for vetted professionals, Nestling connects families with caregivers such as postpartum doulas, lactation consultants, and infant care specialists. These experts can assist with tasks like meal prep, light housekeeping, and overnight care, giving you the time and space to focus on bonding with your baby. With background checks, verified certifications, and flexible booking options, you can access tailored support - whether you need help with breastfeeding, emotional recovery, or sleep training.
It’s worth noting that 72% of postpartum parents feel unsure about their caregiving abilities. Working with a professional who can teach you to read your baby’s cues and offer evidence-based advice can significantly boost your confidence during this vulnerable time.
Prioritize Sleep Hygiene and Self-Care
Sleep deprivation can take a toll on emotional resilience, often worsening postpartum depression symptoms. Dr. Sue Varma from NYU Langone Health highlights the essentials for recovery:
Sleep, rest, help with the baby, good communication and a supportive partner, are the basics in the recovery period for all new moms.
Simple tweaks to your sleep habits and self-care routine can make a world of difference. By focusing on better sleep, gentle movement, and balanced nutrition, you can strengthen your emotional well-being.
Improve Sleep Quality
Getting quality sleep is crucial for emotional recovery, even if it comes in short bursts. Try resting whenever your baby sleeps - those small naps can add up. Work with your partner or a trusted caregiver to take turns so each of you gets at least one solid block of uninterrupted sleep. Make your sleep environment as restful as possible by keeping it dark, cool, and quiet. Start your mornings with exposure to natural light and practice slow, deep breathing to set a calm tone for the day.
If you find yourself unable to fall asleep within 15–20 minutes, leave your bed and do something soothing, like reading or listening to calming music. Preparing for nighttime wake-ups can also help - keep essentials like water, snacks, and burp cloths handy by your feeding spot. To wind down before bed, unplug from electronics and avoid watching the news one to two hours beforehand. Also, steer clear of caffeine after noon and skip alcohol close to bedtime.
For families needing extra help, services like Nestling provide overnight caregivers who can handle night feedings and diaper changes, giving you the chance to recharge during those early, demanding weeks.
Do Gentle Physical Activity
In addition to sleep, gentle physical activity can lift your mood and boost your energy. Even a short walk can make a difference - just 30 minutes of walking daily can improve how you feel. If you're starting out, aim for five to 10 minutes of light movement, such as a relaxed stroll, simple stretches, or pelvic floor breathing, once your healthcare provider gives the green light. Mindful walking - where you focus on your breath and surroundings - can be particularly grounding. Phoenix Health explains:
Each time that you 'catch' a negative thought and bring yourself back [during activity], you are building emotional strength.
Even spending a few moments in morning sunlight, whether outside or by an open window, can help stabilize your mood for the day ahead.
Maintain a Balanced Diet
Eating well is another key to recovery, helping regulate hormones, support milk production, and reduce stress. Focus on whole, nutrient-rich foods like fruits, vegetables, lean proteins, and whole grains. Pairing carbohydrates with protein or healthy fats can help keep your blood sugar steady and your energy levels consistent. If cooking feels overwhelming, opt for simple solutions like one-pan meals, frozen veggies, or using hummus as a quick pasta sauce.
Staying hydrated is just as important. A practical tip: drink a full glass of water every time you feed your baby to ensure you're getting enough fluids. Feeling too stretched to cook? Organize a meal train with friends or explore meal delivery services. Proper nutrition and hydration not only ease physical exhaustion but also help reduce postpartum depression symptoms.
Know When to Seek Professional Help
While self-care, mindfulness, and leaning on friends or family are vital, there are times when professional help becomes necessary. Recognizing when to seek that help can be a pivotal step in your recovery process.
Recognize Signs of Postpartum Anxiety or Depression
If feelings of sadness, anxiety, or emptiness linger beyond two weeks or grow more intense, it’s time to reach out for help. Be on the lookout for signs like persistent sadness, hopelessness, irritability, withdrawal from activities, trouble concentrating, difficulty bonding with your baby, or doubts about your ability to care for them.
In urgent situations - such as thoughts of self-harm, harming your baby, overwhelming despair, or symptoms of postpartum psychosis (like hallucinations or delusions) - call 988 or 911 immediately. You can also contact the National Maternal Mental Health Hotline at 1-833-TLC-MAMA (1-833-852-6262) for 24/7 support.
Postpartum depression affects about 15% of mothers, often starting between 4 to 8 weeks after childbirth, though symptoms can appear as late as six months postpartum. The National Institute of Mental Health stresses:
Perinatal depression is a medical condition that can affect any pregnant or postpartum woman, regardless of age, race, ethnicity, income, or education.
Your doctor may also check for physical issues like anemia or thyroid problems, which can mimic or worsen symptoms of depression.
Consider Therapeutic Options
When self-care and support from loved ones aren’t enough, professional therapies can provide the extra care you need. Evidence-based approaches, such as Cognitive Behavioral Therapy (CBT) and Interpersonal Therapy (IPT), are designed to address negative thought patterns and strengthen your support system. Medication can also be an option, with some benefits - like improved sleep or appetite - showing up before the medication reaches its full effect in 4 to 8 weeks. For more severe cases, treatments like zuranolone (a pill) or brexanolone (an IV infusion), approved by the FDA for postpartum depression, may offer faster relief than traditional antidepressants.
If you’re unsure where to start, your OB/GYN or primary care provider can connect you with a mental health professional. If you’ve experienced depression in the past, consider identifying a psychiatrist or therapist before your delivery, so you have a plan in place if symptoms arise again.
Combining therapy with practical, in-home support can further ease the challenges of this time.
Use Professional Services for Stress Reduction
Professional services can significantly lighten the load of caring for a newborn. Lactation consultants, postpartum doulas, and infant care specialists can help with feeding, overnight care, and even household tasks, reducing stress and allowing you to focus on recovery. Mental health challenges affect at least 1 in 5 mothers, yet about 75% of those affected don’t receive the care they need.
Nestling offers a solution by connecting you with trusted postpartum professionals, including doulas, lactation consultants, and infant care specialists. These experts provide services tailored to your needs, whether it’s overnight care to help you get some much-needed rest, feeding support to reduce anxiety, or assistance with daily tasks. By addressing these challenges early, professional support can prevent minor issues from becoming overwhelming. With flexible scheduling and personalized care plans, Nestling makes it easier to get the help you need, exactly when you need it.
Conclusion
Postpartum resilience isn’t about striving for perfection - it’s about equipping yourself with the tools to navigate challenging emotions and situations. By leaning on practical, evidence-backed strategies, you can create a strong foundation for mental well-being during the fourth trimester and beyond.
Practicing mindfulness, like controlled breathing, can help you stay grounded when emotions run high. Building a solid support network - whether through family, friends, or postpartum groups - can ease the feelings of stress and isolation that often accompany this period. Equally important is prioritizing rest and self-care, as quality sleep plays a crucial role in maintaining emotional balance. Together, these approaches enhance your ability to face each new challenge with confidence.
It’s worth noting that perinatal mental health conditions affect over 20% of women during pregnancy and in the first year postpartum. Seeking professional support, whether through therapy, medication, or services like vetted newborn care services, is a proactive step toward nurturing your mental health. Taking these steps lays the groundwork for long-term resilience.
"Developing postpartum resilience isn't about eliminating difficult emotions but finding effective ways to manage them." - Phoenix Health
Your well-being is deeply connected to your ability to care for your baby and yourself. By combining these strategies and seeking support when needed, you can build the resilience to not just manage but thrive during the postpartum journey.
FAQs
How do I know if my postpartum emotions are normal or if I should seek help?
It’s normal to feel a rollercoaster of emotions - mood swings, tearfulness, anxiety, and even trouble sleeping - shortly after giving birth. These are often called the "baby blues" and usually fade within a week or two. But if those feelings stick around, get worse, or start to include things like hopelessness, trouble taking care of yourself or your baby, or major disruptions to your daily life, it’s important to talk to a healthcare professional.
Reaching out sooner rather than later can make a huge difference. Postpartum emotional challenges don’t mean you’ve failed or that you’re weak - help is out there to support you through this period. You’re not alone.
What are some easy mindfulness techniques I can use daily as a new mom?
Mindfulness doesn’t have to be a time-consuming practice, especially when you’re navigating life with a newborn. Here are a few easy ways to weave mindfulness into your daily routine:
- Pause and breathe: As you hold your baby, take a deep breath in for 4 seconds, then slowly exhale for 6 seconds. Pay attention to the gentle movement of your chest and your baby’s as you breathe together.
- Mindful diaper changes: During diaper changes, focus on the moment. Notice the texture of the wipes, the warmth of your baby’s skin, and the little sounds they make. Let go of distractions and be fully present with your baby.
- Gratitude moments: At the end of the day, take a few seconds to reflect on three things you’re thankful for. It could be your baby’s steady heartbeat, their tiny fingers, or the peacefulness of the evening.
These simple practices can help you feel more connected and grounded, even during the whirlwind of motherhood.
How can I communicate my needs to my support system after having a baby?
Expressing your needs clearly plays a crucial role in building emotional resilience during the postpartum period. Start by tuning into your emotions and pinpointing the type of support you need. Maybe it’s extra rest, help with feeding, or just a few moments of quiet. Be gentle with yourself - it’s perfectly normal and healthy to ask for help as part of your recovery.
When communicating your needs, try using "I" statements to keep the focus on your feelings, paired with a specific request. For instance: "I’m feeling really exhausted and could use a 30-minute nap. Would you mind watching the baby while I rest?" Keeping these conversations brief and distraction-free - or even jotting down your priorities - can help minimize misunderstandings and ensure everyone is aligned.
If you find you need more support, professional postpartum services can be incredibly helpful. For example, Nestling connects families with experienced caregivers like postpartum doulas and lactation consultants. These professionals offer customized assistance with newborn care, emotional support, and more. You’re not alone in this journey, and building a reliable support system is an important step toward recovery and overall well-being.










