Breastfeeding Problems: Common Issues Answered

Breastfeeding Problems: Common Issues Answered
Breastfeeding is natural but not always easy. Many mothers face challenges like latching issues, nipple pain, and milk supply concerns, especially in the early days. Here's a quick overview of common problems and solutions:
- Latching Problems: Nearly 50% of babies struggle to latch properly on day one. Signs include sharp pain, clicking sounds, or flattened nipples. Solutions include trying different breastfeeding positions like cross-cradle or football hold and seeking help from lactation consultants.
- Nipple Pain: Up to 90% of mothers experience soreness, but severe pain or bleeding could signal improper latching or infections like mastitis or thrush. Addressing latch issues and using treatments like lanolin cream or hydrogel pads can help.
- Milk Supply Concerns: Low supply often stems from infrequent feedings or poor milk removal, while oversupply can cause discomfort and fast letdowns. Nursing frequently, staying hydrated, and adjusting techniques can balance supply.
- Engorgement: Painful swelling is common in the first week. Feeding on demand, using cold compresses, and softening the areola before latching can relieve symptoms.
- Infections: Mastitis and thrush require prompt care. Symptoms like fever, red streaks, or shiny, flaky nipples should be addressed with medical advice.
If breastfeeding feels overwhelming, don’t hesitate to seek help. Lactation consultants, postpartum doulas, and support groups can provide guidance and emotional support. Early intervention can make breastfeeding more comfortable and sustainable.
Breastfeeding Issues & Solutions | Ask an Expert
sbb-itb-9ce2258
Latching and Positioning Problems
Getting the hang of latching and positioning is a big step in tackling early breastfeeding hurdles. It’s not always easy at first, but with a little guidance, you can make feeding more comfortable and effective for both you and your baby.
A proper latch is key to successful breastfeeding. When your baby latches correctly, they can feed efficiently, and you can avoid painful nipple issues. However, about 50% of babies have trouble latching on their first day of life. This makes it essential for new moms to spot and address latching problems early.
How to Tell If Your Baby Has a Poor Latch
Once breastfeeding is established, a good latch should feel comfortable. As Dr. Jane Morton puts it, "Pain is really a sign that something is wrong. Nature would not design a system where it hurts to feed a baby". Signs of a poor latch include sharp or pinching pain, clicking or smacking sounds during feeding, dimpled cheeks, and flattened nipples after nursing.
On the other hand, a proper latch looks and feels different. Your baby’s mouth will be wide open, their lips flanged outward like "fish lips", and their chin will press firmly against your breast. You should hear rhythmic swallowing, not clicking. If your baby loses more than 10% of their birth weight, it could mean they’re not transferring milk effectively.
Best Breastfeeding Positions to Try
Finding the right breastfeeding position can make latching easier and more comfortable. In every position, make sure your baby’s head, shoulders, and hips are aligned with their body pressed close to you. Using the "nose to nip" technique - aiming your nipple at your baby’s nose - encourages them to tilt their head back and open wide for a deeper latch.
- Laid-back (reclining) positions: Perfect for the early weeks, this position uses gravity to help your baby latch deeply. Recline at about a 45-degree angle with your baby lying belly-down on your chest.
- Cross-cradle hold: Ideal for beginners, this position gives you more control over your baby’s head. Use the hand opposite the breast you’re feeding from to support their head.
- Football (clutch) hold: A great option if you’ve had a C-section, as it keeps your baby away from your incision.
- Side-lying position: Perfect for night feedings or when you need rest. Lie on your side facing your baby, making it easy for both of you to relax while nursing.
If latching becomes painful, gently break the latch by inserting a clean finger into the corner of your baby’s mouth before trying again. Good positioning not only improves latch quality but also reduces discomfort, which is a topic we’ll explore further.
Physical Issues That Affect Breastfeeding
Sometimes, physical conditions make latching more challenging. One common issue is tongue-tie (ankyloglossia), where a tight frenulum limits tongue movement. This can lead to shallow latches, nipple pain, and poor milk transfer.
Flat or inverted nipples can also complicate the initial latch, but they don’t prevent breastfeeding. As Genevieve Thomas, IBCLC at UCLA Health, explains: "Babies don’t nipple feed. They breastfeed. It doesn’t matter if the nipple is sticking out or not with breastfeeding because we’re not sticking nipples into a baby’s mouth like we might with bottle feeding". The key is for your baby to latch onto the breast tissue, not just the nipple. Techniques like skin-to-skin contact and the football hold can encourage your baby to latch deeply, and over time, natural suction often helps the nipple protrude more.
Severe engorgement can also make latching harder by flattening the nipple and firming up the areola. In this case, try reverse pressure softening - apply firm inward pressure toward your chest for about 50 seconds to move fluid back and soften the area before feeding.
If you suspect issues like tongue-tie, weak sucking, or other physical challenges, consult a lactation consultant or pediatrician for personalized advice. Addressing these concerns early on can make a big difference in your breastfeeding journey.
Nipple Pain and Breast Infections
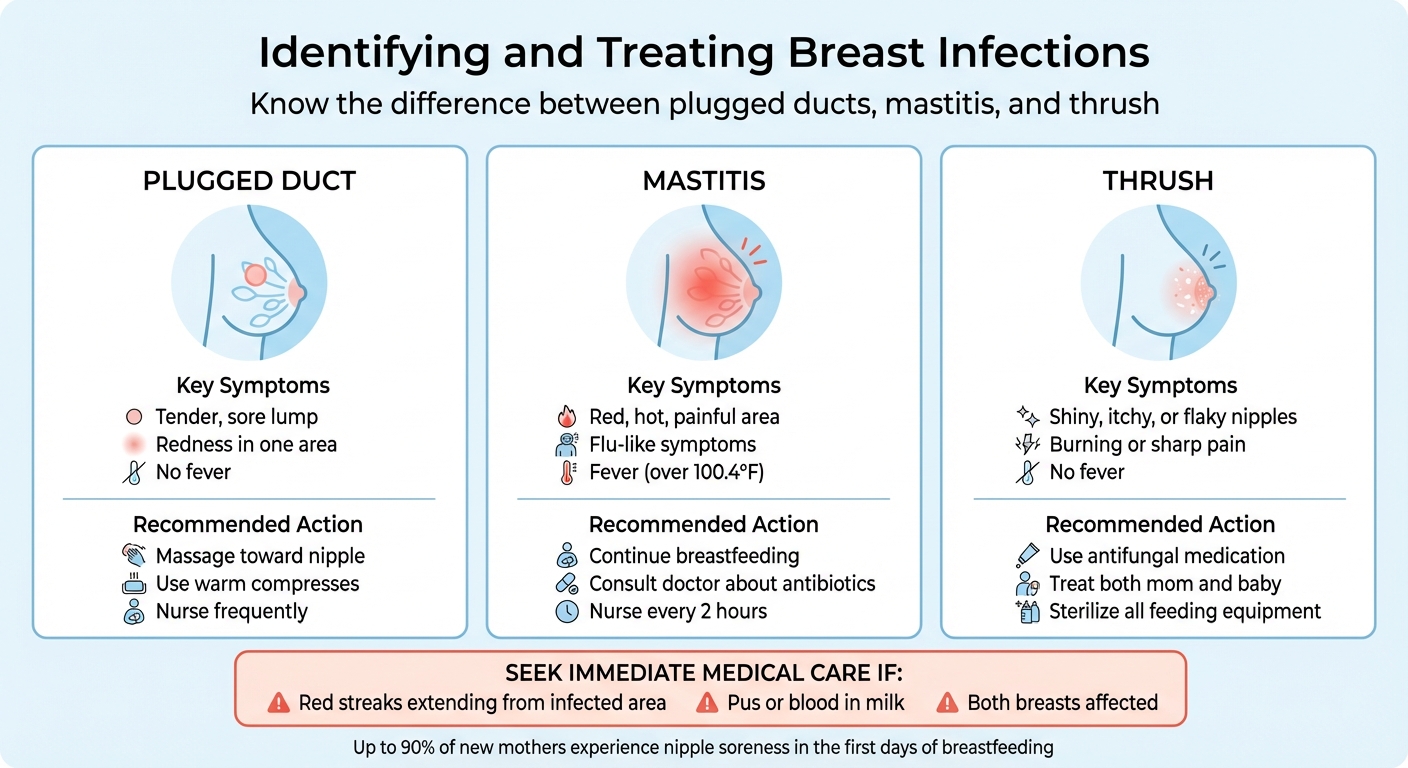
Breast Infection Types: Symptoms and Treatment Guide
Nipple pain is a common challenge many mothers face, often leading them to consider stopping breastfeeding. Knowing the difference between normal discomfort and signs of a more serious issue can help you address problems early and stay on track with your breastfeeding journey.
Normal Soreness vs. Serious Pain
Up to 90% of new mothers report some level of nipple soreness during the first days of breastfeeding. This type of soreness is usually temporary, peaking around the fifth day as your body adjusts. It often feels like mild tenderness or sensitivity when your baby latches and typically eases as the feeding continues.
However, pain that is sharp, burning, or shooting - and lasts beyond seven days - could signal a bigger problem. Symptoms like bleeding, deep cracks, or fever might point to an improper latch, an infection, or other complications. These issues should be evaluated by a healthcare professional.
How to Prevent and Heal Nipple Damage
Start by ensuring your baby latches onto a large portion of the breast, not just the nipple. When it’s time to end a feeding, avoid pulling your baby off the breast directly. Instead, gently insert a clean finger into the corner of their mouth to break the suction.
After nursing, applying a few drops of breast milk to your nipples can help soothe and protect the skin. Let your nipples air dry completely before putting on a bra or nursing pads, as moisture can lead to irritation or infection.
For cracked or sore nipples, consider using purified lanolin cream to create a protective barrier, or try hydrogel pads for a cooling effect and to reduce friction. Avoid using harsh soaps, alcohol, or astringents on your nipples; plain water is enough to clean them while maintaining your skin’s natural oils.
Switching up breastfeeding positions and wearing a supportive cotton bra can also help by easing pressure on the nipples and promoting proper milk flow.
While prevention is important, it’s equally critical to address infections quickly if they occur.
Treating Breast Infections
Breast infections causing pain generally fall into three categories: plugged ducts, mastitis, and thrush. Each requires a specific treatment approach.
| Condition | Key Symptoms | Fever Present? | Recommended Action |
|---|---|---|---|
| Plugged Duct | Tender, sore lump; redness in one area | No | Massage toward the nipple, use warm compresses, and nurse frequently |
| Mastitis | Red, hot, painful area; flu-like symptoms | Yes (over 100.4°F) | Continue breastfeeding and consult your doctor about antibiotics |
| Thrush | Shiny, itchy, or flaky nipples; pain | No | Use antifungal medication for both mom and baby |
Mastitis is a bacterial infection that causes redness, heat, and tenderness in one area of the breast, often accompanied by fever, chills, and body aches. If symptoms persist beyond 12–24 hours, contact your doctor for antibiotics. Keep breastfeeding from the affected side every two hours to maintain milk flow - your milk is safe for your baby even during an infection. Warm compresses and gentle massage toward the nipple can ease discomfort, and positioning your baby so their chin points toward the tender area may help clear the blockage.
Thrush, a fungal infection, can cause burning, itching, and sharp pain in the breast, often during or after feedings. Nipples may appear shiny, pink, flaky, or blistered. To effectively treat thrush, both you and your baby need antifungal medication to avoid re-infection. During treatment, sterilize breast pump parts, pacifiers, and bottle nipples by boiling them for 10 minutes daily. Wash towels and clothing in water hotter than 122°F to eliminate yeast.
If you notice red streaks extending from the infected area, pus or blood in your milk, or if both breasts appear affected, seek immediate medical care. These symptoms could indicate a more serious condition requiring urgent attention.
Milk Supply and Engorgement Issues
Concerns about milk production can often lead to increased stress. Gaining a clear understanding of your milk supply and addressing any genuine concerns can help you feel more at ease and in control.
What Low Milk Supply Really Means
Low milk supply refers to producing less milk than your baby needs. However, many mothers worry about their supply when, in reality, everything is functioning as it should. The key lies in observing measurable signs rather than relying on how your breasts feel.
By day 4, look for at least 6 wet diapers and 3 poopy diapers daily; steady weight gain is another reliable indicator of an adequate milk supply. If your baby is meeting these milestones, your supply is likely sufficient - even if your breasts feel softer or no longer leak. Over time, it’s normal for breasts to feel less full, and frequent nursing or cluster feeding is part of the process.
True low milk supply is often linked to factors like infrequent feedings, a poor latch that prevents effective milk removal, or underlying medical conditions such as Polycystic Ovary Syndrome (PCOS), hypothyroidism, or previous breast surgeries. Certain medications, including some birth control methods, decongestants, and antihistamines, can also affect milk production.
"The principle of supply and demand applies to breastfeeding. The more your baby nurses, the more milk your body will produce." - Tallahassee Memorial HealthCare
To encourage milk production, aim to nurse 8–12 times a day, every 1.5–3 hours, ensuring a deep latch and using breast compression. You can also try 20-minute sessions with a double-electric pump or power pumping (20 minutes pumping, 10 minutes rest, then repeat). Skin-to-skin contact and staying hydrated by drinking 8 to 10 glasses of water daily are also helpful for maintaining lactation.
| Feature | Actual Low Supply | Perceived Low Supply (Normal) |
|---|---|---|
| Weight Gain | Baby is not gaining or is losing weight | Baby is gaining weight steadily |
| Diaper Count | Fewer than 6 wet diapers/day after day 4 | 6+ wet diapers and 3+ poopy diapers/day |
| Breast Sensation | Breasts may never feel full or leak | Breasts feel softer over time |
| Baby Behavior | Baby does not seem to swallow during feeds | Baby nurses frequently or in "clusters" |
Next, let’s explore how to manage engorgement while keeping milk supply balanced.
How to Relieve Engorgement
Engorgement happens when milk builds up in the breasts, usually lasting 24–48 hours. This swelling occurs as breast tissue fills with fluid.
The best way to manage engorgement is through frequent, on-demand feeding. Express just enough milk to soften the areola for a better latch or to ease discomfort - avoiding full emptying, which can signal your body to produce even more milk.
Reverse pressure softening can help: press the areola inward for 60 seconds to shift fluid away, and hand-express a small amount if necessary to aid latching. Between feedings, cold compresses or ice packs wrapped in a cloth can reduce swelling and pain when applied for 10 to 20 minutes. Gentle strokes from the nipple toward the armpit can also encourage drainage.
Wearing a supportive, well-fitting bra without underwire can prevent milk duct constriction. Over-the-counter pain relievers like ibuprofen can help manage inflammation and discomfort. If you notice symptoms like a fever over 100.4°F, red streaks on your breast, or if your baby struggles to latch, contact your healthcare provider - these could indicate mastitis.
If your milk supply exceeds your baby’s needs, a different approach is required.
Dealing with Too Much Milk
Having an oversupply can bring its own set of challenges. A fast letdown can cause your baby to cough, choke, or bite, and might result in frothy stools and frequent hunger. For mothers, it can lead to discomfort, leaking, blocked ducts, and recurrent mastitis.
Generally, milk supply stabilizes around four to six weeks postpartum as prolactin levels adjust to your baby’s needs. To manage an overactive letdown, try nursing in a reclined or side-lying position to slow the milk flow, giving your baby more control. If your baby chokes during feeding, unlatch them and let the initial spray fall into a towel before re-latching. You can also use the "scissor hold", gently pressing the nipple between your first and middle fingers to reduce the force of the letdown.
For chronic oversupply, block feeding can help. This involves nursing from only one breast for a set period - such as four hours - to signal your body to slow milk production. Avoid continuing block feeding for more than five days. Pump or hand express just enough to relieve discomfort, as excessive pumping can encourage more production. Additionally, it’s wise to stop using lactation teas, cookies, or herbal supplements designed to increase supply.
Adjusting your nursing techniques and positions can make a big difference, ensuring both you and your baby find comfort while maintaining a healthy milk supply.
Emotional Support and Practical Advice
Navigating the emotional challenges of breastfeeding is just as important as addressing the physical ones. Many mothers face feelings of frustration and guilt during this time, especially when difficulties arise. A study involving 422 mother–infant pairs highlighted that issues like cracked or sore nipples, low milk supply, and breast engorgement are some of the most common stressors during the first month postpartum. It’s important to remember that breastfeeding is a skill you learn over time, not something that comes naturally to everyone. Giving yourself the grace to learn can help ease some of the pressure.
Managing Breastfeeding Stress and Frustration
Taking small steps each day can help build your confidence. Physical challenges, such as nipple pain or trouble with latching, can add to your stress, so seeking professional help to address these issues is crucial. Self-care is equally important. Eating nutritious meals, staying hydrated, and resting whenever possible can improve both your mood and milk supply. Don’t hesitate to delegate household chores so you can focus on recovery and feeding.
"Remember, help is available and there are solutions." - WIC Breastfeeding Support
Creating a calm environment can also make a difference. Nursing in a quiet, dimly lit space and maintaining skin-to-skin contact can encourage milk let-down and strengthen your bond with your baby. Building a strong support system - whether through your partner, family, or professionals - can significantly enhance your breastfeeding experience. Lactation experts and caregivers can provide hands-on assistance to make the process smoother.
Getting Help from Postpartum Caregivers
Postpartum doulas and lactation consultants can be invaluable during this time, offering hands-on help with feeding techniques, physical recovery, and establishing daily routines. Certified lactation consultants specialize in addressing latching difficulties, milk supply concerns, and infections. Postpartum doulas provide well-rounded support, including emotional encouragement, newborn care, and even light household tasks, allowing you to focus on healing and bonding with your baby .
"Postpartum care supports parents in resting, recovering, and adjusting to newborn life." - Maternal Instincts
If you’re dealing with issues like plugged ducts or mastitis, taking extra time to rest is essential. Delegating chores can give you the breathing room you need to recover . It’s also a good idea to contact a lactation consultant or midwife at the first sign of pain or latch issues to prevent complications from worsening . Joining a support group, such as La Leche League, or connecting with WIC peer counselors can also provide emotional support and the chance to share experiences with others who understand .
In addition to traditional caregiving, modern solutions now combine expert guidance with practical services.
How Nestling Supports Breastfeeding Families
Nestling is a platform that connects families with trusted lactation consultants and infant care specialists who provide personalized guidance. Whether you’re dealing with latching problems, nipple pain, engorgement, or mastitis, Nestling helps create customized breastfeeding plans tailored to your needs. Beyond clinical care, the platform also offers access to postpartum doulas who can assist with newborn routines, emotional recovery, and light household tasks - easing your workload during those early weeks. With flexible booking options, backup care availability, secure payment systems, and ongoing feedback, Nestling ensures you have compassionate, reliable support throughout your breastfeeding journey.
Conclusion: Getting the Right Help for Breastfeeding Success
Getting timely assistance can address common breastfeeding challenges before they turn into more serious issues. Many mothers stop breastfeeding before the six-month mark due to these difficulties. Taking action early can set the stage for a more manageable breastfeeding experience.
"If you find yourself putting off feedings because breastfeeding is painful, get help from a lactation consultant. Delaying feedings can cause more pain and harm your milk supply." - U.S. Department of Health & Human Services
Don’t wait if you notice any concerns. Whether breastfeeding is painful or your baby seems unsatisfied after feeding, reach out to a midwife, health visitor, or lactation consultant right away. Early intervention not only helps prevent conditions like mastitis but also boosts your confidence during those early postpartum weeks.
"With guidance and support as well as appropriate medical treatment when needed, it is usually possible to overcome these obstacles and continue breastfeeding for a longer time." - UpToDate
Professional support is essential for navigating breastfeeding challenges. You can contact resources like the OWH Helpline (1-800-994-9662), WIC breastfeeding experts, or platforms such as Nestling to connect with certified lactation consultants and postpartum doulas. These specialists can tailor care plans to your needs, helping you overcome obstacles and create a breastfeeding routine that works for you. With the right guidance, you can build a more comfortable and lasting breastfeeding experience.
FAQs
How do I know if my baby is latching properly during breastfeeding?
A proper latch is essential for both comfortable and effective breastfeeding. Here's how you can tell if your baby is latched on correctly:
- Mouth position: Your baby’s mouth should be wide open, with their chin touching your breast. Most of the areola, not just the nipple, should be inside their mouth.
- Lip placement: Their lips should be turned outward, like a little fish.
- Cheek and body alignment: Rounded cheeks are a good sign, and their chest and tummy should be snug against your body.
- Comfort: Breastfeeding shouldn’t hurt. If you feel pain or discomfort, it might mean the latch needs some adjustment.
If you’re having trouble or feel unsure, don’t hesitate to contact a lactation consultant. They can provide expert advice tailored to you and your baby. Keep in mind, every mother and baby duo is different, and finding the perfect latch may take a little time and practice!
What should I do if I think I have a breast infection?
If you suspect you have a breast infection, reach out to your healthcare provider as soon as possible for an evaluation. They may recommend antibiotics to address the infection, and in most cases, you can keep breastfeeding while undergoing treatment.
To help with discomfort, consider using over-the-counter pain relievers as instructed and applying warm compresses to the affected area. Make sure to get plenty of rest, drink enough fluids, and nurse or pump regularly to reduce engorgement and maintain milk flow. If your symptoms get worse or don’t start improving, be sure to follow up with your doctor without delay.
What can I do to manage an oversupply of breast milk?
If you’re producing more breast milk than your baby needs, there are a few ways to manage the situation. One approach is to nurse from only one breast during each feeding. This can help regulate your supply to better match your baby’s needs. Be cautious with pumping - doing it too often might encourage your body to produce even more milk. If you’re feeling overly full, try gently hand-expressing just enough milk to ease the discomfort. You can also use breast compression during nursing to slow the milk flow, making feedings more comfortable for your baby.
For relief from engorgement, applying a cold compress or chilled cabbage leaves between feedings can help reduce swelling and ease discomfort. If managing oversupply feels overwhelming, consider consulting with a lactation expert who can provide tailored guidance and support.










