When To Start Postpartum Cardio Workouts

When To Start Postpartum Cardio Workouts
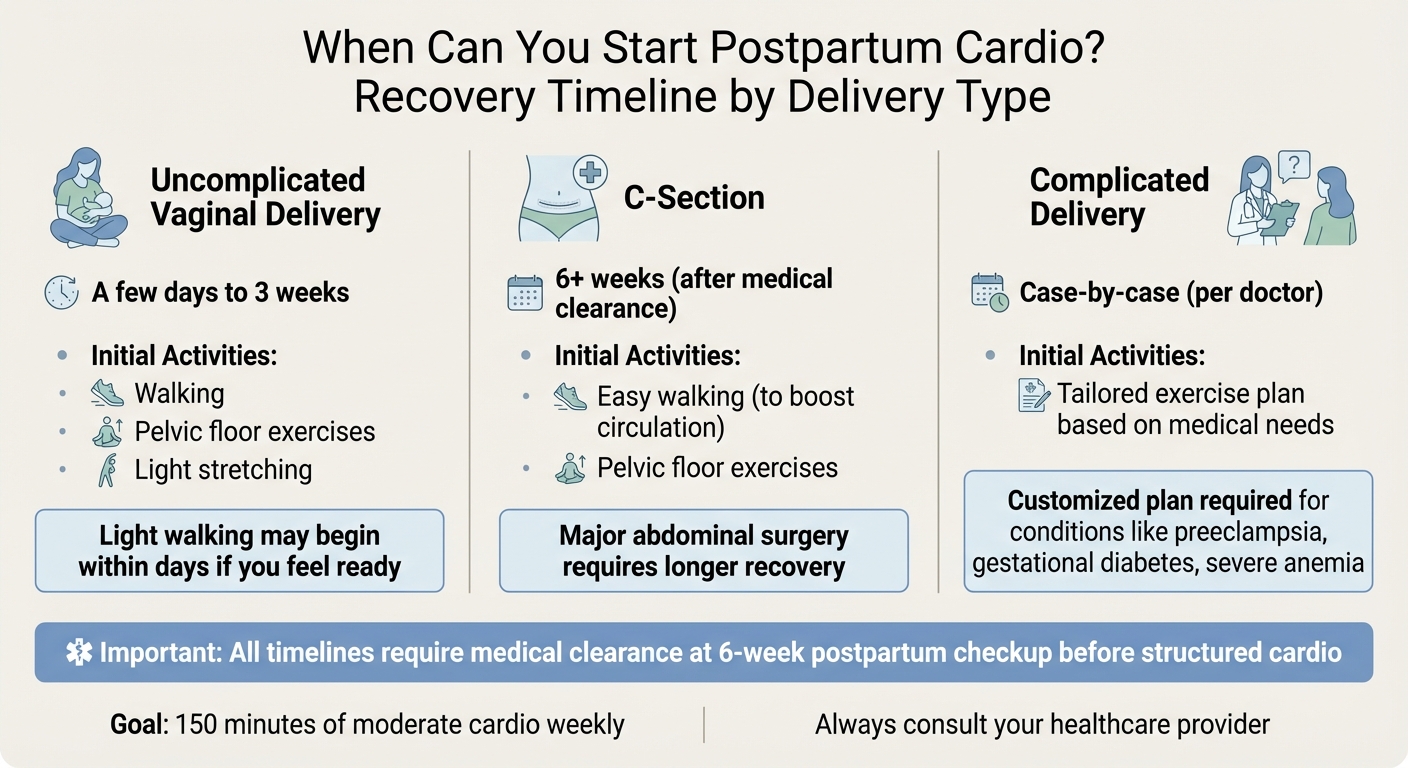
You can safely start postpartum cardio after getting medical clearance, which typically happens around six weeks postpartum for most women. Recovery timelines depend on your delivery type:
- Uncomplicated vaginal delivery: Light walking may begin within days if you feel ready.
- C-section: Wait at least six weeks for structured cardio; gentle walking can start earlier.
- Complicated delivery: Follow a custom plan from your doctor.
Key tips:
- Aim for 150 minutes of moderate cardio weekly (e.g., walking, cycling, or swimming).
- Watch for warning signs like pain, bleeding, or pelvic heaviness - stop and consult your doctor if these occur.
- Focus on gradual progress and listen to your body; mental readiness is as important as physical.
Always prioritize recovery and consult your healthcare provider for personalized guidance.
Postpartum Cardio Workout | Intro Back Into Cardio
sbb-itb-9ce2258
Getting Medical Clearance Before Starting Cardio
Postpartum Cardio Start Timeline by Delivery Type
Before diving back into cardio workouts, it’s crucial to get your doctor’s approval. Your healthcare provider will assess how well your body has healed - focusing on areas like C‑section incisions, perineal tears, and pelvic floor recovery - to confirm it’s safe to exercise again. This evaluation can also help identify any serious issues, such as deep vein thrombosis (signaled by calf pain or swelling) or persistent high blood pressure exceeding 140/90 mmHg.
Postpartum recovery is a delicate process. The hormone relaxin, which softens joints and ligaments during pregnancy, can linger, raising the risk of injury. Overexertion too soon might lead to complications like vaginal bleeding, uterine prolapse, or worsening diastasis recti.
The American College of Obstetricians and Gynecologists (ACOG) underscores the importance of this step:
A thorough clinical evaluation should be conducted before recommending an exercise program to ensure that a patient does not have a medical reason to avoid exercise.
Once you’ve received medical clearance, it’s time to consider how your recovery timeline will vary based on your delivery type.
Recovery Timelines by Delivery Type
Your delivery experience plays a big role in determining when you can safely ease back into cardio. For those who had an uncomplicated vaginal delivery, light activities like walking or gentle stretching can often begin just days after giving birth - whenever you feel ready.
C‑sections, on the other hand, require a longer recovery. Since this procedure is major abdominal surgery, it takes weeks for the incision to heal enough to handle structured exercise. While formal cardio might need to wait until around six weeks postpartum, gentle walking is encouraged early on to support healing and reduce the risk of blood clots.
Dr. Christie Cobb, a board-certified OB/GYN, explains why recovery timelines aren’t one-size-fits-all:
I believe the absence of an absolute timeline from ACOG for resuming exercise postpartum is based on the recognition of individual needs.
For women with more complicated deliveries - such as those involving gestational diabetes, preeclampsia, or severe anemia - exercise plans should be customized by their healthcare provider. Additionally, over 60% of pregnant and postpartum women report low back pain, which can worsen if exercises aren’t done properly.
| Delivery Type | Typical Cardio Start Timeline | Recommended Initial Activities |
|---|---|---|
| Uncomplicated Vaginal | A few days to 3 weeks | Walking, pelvic floor exercises, light stretching |
| C‑Section | 6+ weeks (after medical clearance) | Easy walking (to boost circulation), pelvic floor exercises |
| Complicated Delivery | Case‑by‑case (per doctor) | Tailored exercise plan based on medical needs |
For all delivery types, the six-week postpartum checkup serves as the key milestone for transitioning into structured cardio routines.
The 6‑Week Postpartum Checkup
This appointment is a key moment for getting the go-ahead to return to exercise. At the six-week checkup, your doctor will evaluate how your uterus, cervix, and any incisions or tears have healed. They’ll also check for conditions like diastasis recti or pelvic floor dysfunction, which might require treatment from a pelvic floor physical therapist before engaging in high-impact cardio.
Once cleared, this checkup often marks the green light for more strenuous cardio and moderate-intensity workouts. As Dr. Christie Cobb notes:
Six weeks is a good general timeline for resuming exercise, with some gentle walking being possible before then.
For C‑section moms, this visit is especially critical to ensure both internal and external incisions have healed enough to handle the abdominal pressure that cardio can create. Be prepared to discuss any symptoms like leaking, pelvic heaviness, or abdominal "coning." If you’re aiming to return to high-impact activities like running, ask your doctor about specific benchmarks to hit before increasing intensity. You might also want to request a referral to a pelvic floor physical therapist if you’re concerned about core or pelvic stability.
Signs You're Ready to Start Cardio
After getting the green light from your doctor, your body will give you clues about whether it's ready for cardio. Paying attention to these physical and emotional signals can help you avoid setbacks and ease into recovery.
Physical Signs of Readiness
Your body should handle daily activities - like walking, carrying your baby, and household chores - without any pain in your pelvis, abdomen, joints, or vaginal area. If you feel discomfort during these tasks, it’s a sign your body needs more time.
Pelvic floor stability is another key indicator. Studies show that one in three women experience involuntary urine leakage within the first three months postpartum. If you notice incontinence or a feeling of heaviness in your pelvic area, it’s best to wait. Heather Jeffcoat, a pelvic health physical therapist, emphasizes:
Stop whatever you're doing and see a pelvic health physical therapist if you experience any leakage, signs of prolapse (pelvic heaviness or pressure), back or joint pain.
Pay attention to your lochia (postpartum bleeding). If light activity causes it to increase or turn bright red, hold off on cardio. Another readiness marker is being able to walk for 10 to 30 minutes without feeling wiped out.
Check for diastasis recti by engaging your abdominal muscles. If you notice "coning" (a bulging appearance along your midline), it might indicate this condition, which affects up to 60% of women six weeks postpartum. Additionally, monitor your morning resting heart rate. If it’s elevated by more than 10 beats per minute, your body probably needs more rest.
While these physical cues are essential, emotional readiness is just as important.
Emotional and Energy Levels
Feeling physically ready doesn’t mean much if you’re not mentally prepared to return to exercise. Dr. Heather Irobunda, an OB-GYN, advises:
If you find that you don't feel up to it because of exhaustion, listen to your body. Give yourself grace during this period.
Exercise should leave you feeling energized, not drained. If it adds to your stress or feels overwhelming, it’s okay to wait. Dr. Christie Cobb reminds us:
Caring for yourself and a baby and focusing on managing the new balance is rigorous enough.
Sometimes, taking a nap might be a better use of your free time than squeezing in a workout. Sleep deprivation is no joke, and rest can often do more for your recovery than pushing through a workout when you're running on empty. The key is finding a balance - exercise should enhance your well-being, not add to your stress. If you’re dealing with extreme fatigue or emotional struggles, prioritize healing first. Cardio can come later.
Safe Cardio Exercises for New Mothers
Starting with Low-Impact Activities
If you're easing back into fitness after giving birth, walking is an excellent first step. Begin with short 5–10 minute walks soon after an uncomplicated vaginal delivery, gradually adding a minute each day as long as you're pain-free. A simple way to gauge your effort is the "talk test" - you should be able to hold a conversation but not sing a tune.
Another gentle option is stationary cycling, which boosts cardiovascular health without the jarring impact of running. Most new mothers can try this around 4–6 weeks postpartum, but only after getting the green light from their doctor. Similarly, swimming and water aerobics are great for full-body conditioning without stressing your joints. Just ensure your postpartum bleeding (lochia) has stopped and any tears or incisions have fully healed - usually by 4–6 weeks.
Postnatal yoga and Pilates are also worth considering. These activities help rebuild flexibility and core strength while providing light aerobic benefits. If group classes appeal to you, try low-intensity aerobics or dance, including fun "baby-and-me" sessions. Just remember to consult your doctor first and, if you're breastfeeding, pump or feed beforehand to stay comfortable. Staying hydrated and maintaining adequate calorie intake is also key.
Moving to Higher-Intensity Workouts
Once your endurance improves, you can gradually introduce more intense activities. For example, high-impact exercises like running or jogging are best postponed until at least 12 weeks postpartum. This allows your pelvic floor and joints time to stabilize. Pregnancy hormones like relaxin, which loosen ligaments, can linger in your body for 6 to 12 months, leaving your joints more prone to injury. As Dr. Christie Cobb, an OB-GYN, explains:
The joint instability from relaxin released in pregnancy does not magically disappear after delivery.
When you're ready to try jogging - typically around 8–12 weeks postpartum - start with short intervals. For example, jog for 60 seconds, then walk for 120 seconds, and repeat. You might also find it easier on your pelvic floor to perform these intervals on a slight incline rather than flat terrain. Aim to gradually build up to 150 minutes of moderate-intensity aerobic exercise per week, which can be broken into manageable 10-minute sessions.
Pay attention to how your body responds to higher-intensity workouts. Changes in vaginal discharge or an elevated resting heart rate - more than 10 beats per minute above your usual baseline - can signal that you're pushing too hard and need extra rest.
When to Pause or Stop Cardio Exercise
Warning Signs and Risks
Your body has ways of letting you know when it’s time to ease up on your workout routine. One major red flag is vaginal bleeding. If your lochia becomes bright red, flows more heavily, or restarts after it had stopped, it’s a sign that you’re overdoing it and need to take a step back. This is your body’s way of saying, “Slow down.”
Pay close attention to pelvic floor symptoms as well. If you notice a feeling of pressure, aching, or bulging in your vagina, it could indicate pelvic organ prolapse. Similarly, urinary leakage during exercise suggests that adjustments to your routine are necessary. Another warning sign is a visible ridge along your midline during activity, which may point to weak abdominal support.
And let’s be clear: pain is a non-negotiable stop sign. If you experience sharp, intense, or persistent pain in your abdomen or pelvic area, stop immediately and seek guidance. Dr. Heather Irobunda, a board-certified OB-GYN, puts it plainly:
If any workouts or exercises cause intense, sharp, or persistent pain (especially if it's in the abdominal or pelvic regions), stop immediately and consult your medical professional.
Other serious symptoms include sharp chest pain, severe headaches, dizziness, fainting, or unexplained shortness of breath - all of which require you to stop right away. Additionally, calf pain or swelling could point to a blood clot, a serious postpartum complication that demands immediate medical attention. If any of these issues arise, pause your workout and contact your doctor as soon as possible.
When to Contact Your Doctor
Certain symptoms go beyond the typical warning signs and call for immediate medical attention. Your recovery is unique, so staying alert to changes in your body is essential. For example, conditions like postpartum cardiomyopathy, unstable high blood pressure (above 140/90 mmHg), kidney disease, or acute infections with fever require medical clearance before resuming moderate-to-vigorous cardio. Similarly, heavy bleeding, fever, foul-smelling vaginal discharge, persistent headaches, or pain and swelling in one leg are all reasons to contact your healthcare provider without delay.
If you’re feeling more drained than energized after workouts or if your muscles remain sore and shaky for an unusually long time, it’s time to check in with your doctor. Dr. Christie Cobb, a board-certified OB-GYN, offers this reminder to new moms:
Caring for yourself and a baby and focusing on managing the new balance is rigorous enough... If exercise makes [stress] worse, back off.
Every postpartum journey is different. Consulting a healthcare professional ensures your exercise routine aligns with your body’s needs and recovery timeline.
How Nestling Supports Your Postpartum Recovery
Postpartum Doula Help with Exercise Recovery
Getting back into cardio after giving birth can feel overwhelming, especially when you're juggling sleepless nights and nonstop baby care. That’s where Nestling’s postpartum doulas come in. These trained professionals guide you through a gradual recovery process, starting with gentle movements like diaphragmatic breathing and pelvic tilts. As you progress, they help you incorporate more challenging activities, using tools like the "talk test" to ensure you're exercising at a safe, moderate level.
Your doula also provides practical tips, such as scheduling workouts after feeding or pumping to stay comfortable. Plus, they keep an eye out for warning signs like increased bleeding, pain, or exhaustion, advising you to pause or rest if needed. If you're running on empty, they may even suggest prioritizing rest over exercise.
But their support doesn’t stop there - Nestling’s doulas go beyond exercise to offer a well-rounded recovery plan tailored to your unique needs.
Customized Care Plans and Emotional Support
Nestling takes a personalized approach to postpartum recovery, creating care plans that match your delivery type, energy levels, and fitness goals. Whether you’ve had a vaginal birth or a C-section, your plan aligns with your healing timeline and encourages you to work toward 150 minutes of moderate-intensity aerobic activity per week. If that sounds daunting, don’t worry - shorter, 10-minute sessions spread throughout your day can help you ease into the routine.
Physical recovery is only part of the equation. Nestling’s doulas also check in on your emotional well-being, recognizing that mental health plays a big role in how ready you feel to exercise. As the Motherhood Center explains:
Engaging in postpartum exercise offers a myriad of benefits that extend beyond physical fitness, contributing to your overall wellness and enhancing the joys of motherhood.
Your doula ensures you're staying hydrated - especially important for breastfeeding moms - and introduces techniques like "360 breathing" to help you feel more grounded and physically stable. With this kind of holistic care, you’re not just recovering; you’re rebuilding in a way that respects both your body and mind.
Conclusion
Postpartum cardio should align with your body's recovery timeline. Start slow, focusing on low-impact activities, and only move to high-impact cardio after at least 12 weeks postpartum - this applies whether you had a vaginal delivery or a C-section.
Let your body's signals guide your progress. Pay attention to physical cues and milestones before increasing intensity. If you notice increased vaginal bleeding, sharp pain, or extreme fatigue during or after exercise, stop immediately and consult your doctor. These symptoms may indicate that your body needs more time to heal.
The American College of Obstetricians and Gynecologists suggests aiming for 150 minutes of moderate-intensity aerobic activity per week. You can break this into shorter sessions - try 10 minutes at a time - and use the "talk test" to measure intensity. If you can talk but not sing, you're likely at the right level.
Before diving into cardio, focus on rebuilding your core and pelvic floor. Start with diaphragmatic breathing, Kegels, and gentle abdominal exercises. Since about 60% of women experience diastasis recti six weeks postpartum, addressing this early can help reduce the risk of long-term issues.
For tailored advice, consider working with Nestling's postpartum doulas to create a recovery plan that fits your individual needs.
And most importantly, be kind to yourself. As Peloton instructor Robin Arzón wisely says:
Listen to your body, honor where it's at, and give yourself grace throughout this process. You just grew and birthed a whole new human, after all!
FAQs
What signs indicate I should stop postpartum cardio workouts?
During postpartum cardio workouts, it’s crucial to stay in tune with your body. If you notice pain, heavy bleeding, dizziness, shortness of breath, or any other unusual symptoms, stop your workout immediately. These could indicate that your body is either not ready or being pushed too hard.
In such cases, contacting your healthcare provider is essential for proper guidance. Keep in mind, every postpartum recovery is different - so go at a pace that feels comfortable and right for you.
When is it safe to move from low-impact to high-impact cardio after having a baby?
To ease into high-impact cardio postpartum, start with gentle movements like walking, light stretching, or pelvic floor exercises. From there, you can gradually increase the intensity, always letting your body guide you. It’s essential to follow your healthcare provider’s advice - most recommend waiting at least 6–8 weeks after giving birth before diving into more strenuous workouts. However, this timeline can vary depending on your recovery and overall health.
Stay in tune with your body. If you notice discomfort, fatigue, or changes in bleeding, it’s a sign to slow down and adjust your routine. Everyone’s postpartum recovery is different, so focus on healing at your own pace rather than rushing back into intense exercise.
Why do you need medical clearance before starting postpartum cardio workouts?
Before diving into postpartum cardio, it's crucial to get a medical clearance. Your body undergoes significant changes during childbirth, and proper healing takes time. A healthcare provider can evaluate your readiness by considering factors such as the type of delivery you had, any complications, and your overall health.
Jumping back into exercise too early can lead to injuries or other complications, so having professional guidance ensures a safer return to physical activity. Remember to prioritize your health and pay attention to how your body feels as you ease back into a fitness routine.










